It Takes a Village to Raise a Child
It takes a village to raise a child is an old African proverb. It means that a child needs both the immediate and extended family to overcome adverse experiences like trauma and to grow up in a safe and secure environment.
Unfortunately, traditional trauma treatment often only includes the individual child. And if the family is involved, it is only those members of the immediate household living under the same roof.
The extended family of friends, ex-spouses, relatives, or institutions (schools, probation officers, child protective service workers, etc.) are rarely engaged or actively involved. And if they are, their roles and function are not well defined. Therefore, the key questions are: “Why does this happen?” and “How do we overcome this problem?” We use the term “village” interchangeably with the term extended family.
Why a Lack of Extended Family (Village) Involvement?

Using the FST| Family Systems Trauma Model, we examine the top two reasons why there is a currently such a lack of extended family involvement in mental health treatment:
#1- The Fear Factor
Therapists will often state, “Family therapy with just the immediate family scares me to death so if you add the complexity of the extended family, I am really overwhelmed.”
Therapists use treatment modalities that they are comfortable with and have received training in. Personally, in graduate school, all my training from my professors and field instructors involved individual treatment and case management. There was little to no formal family therapy training. As a result, all my cases received individual therapy, until I sought out post-graduate family therapy training. Early in my career, it was the fear factor of failing and lack of family therapy tools that kept me from treating the entire traumatized family and its village. Over the last 32 years of my career, I have seen this same fear factor and lack of family therapy training prevent other trauma specialists from actively involving the extended family.
#2-No Step-by-Step Tools and Clarity of Roles
There is a lack of step-by-step tools once the extended family is engaged and answers to the “now what?” question. I have a room full of six or more people that include relatives, neighbors, friends, or institutions. NOW WHAT? What do I do with all these people and what exactly are their roles in helping the immediate family?
Models like Wraparound are great at providing steps and principles to organize the extended family but short on providing clear next steps once everyone is assembled.
For example, what exactly is the grandparent’s role if the child is violent or aggressive with their daughter (the single parent mom)? Do they come over to the house? Do they call the police and if so when and under what circumstances? Or do they do something else?
FST Village Playbook
Within the FST Model, we use what are called, FST Village Playbooks to clarify everyone’s roles in writing within a who? what? when? where? and how? framework. Pre-determining a plan of action in writing is a must have especially with so many people involved. Imagine what would happen if the quarterback football team and the entire offensive line lacked a written playbook of who does what and when before the game. The result would be utter chaos. This is exactly what the village of extended families experience without a written playbook with clarity of roles.
In a case example, a family therapist, asked me to consult with her stuck case. She had been treating the family for over a year. The 15-year-old child, Leon, was involved in both the juvenile justice system for stealing a car and CPS (child protective services) because he was currently living in a home without utilities or a bed. If these matters were not resolved immediately, Leon and his four younger brothers and sisters would be removed and placed in temporary foster care.
The mother, Mary, was clinically depressed and unable to look for employment and her boyfriend was also unemployed.
As a result of these identified problems, I recommended that we involve the village of the local pastor, biological dad, Mary’s boyfriend, the CPS Worker, the Therapist, and the Juvenile Probation officer in a town meeting format. This format had the goal of focusing on solutions in the here and now (get the utilities on) instead of a therapeutic session that was more psychological.
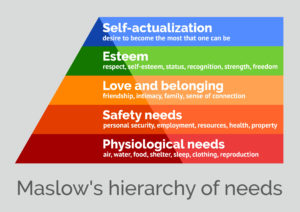
In other words, before any type of psychological counseling could be successful, as Figure 1 illustrates using Maslow’s Hierarchy of Needs, the physiological needs of food, clothing, and shelter had to be addressed first. This is a primary reason why this case had been chronically stuck. The family therapist was: (1) conducting therapy for over a year with just Leon and/or mom. There was no village or extended family involvement; (2) There was psychological counseling around mom’s depression and Leon’s acting out behaviors, but no interventions around basic needs, and (4) there was no pre-written FST Village Playbook to outline a clarity of roles in helping the family address these unmet basic needs.
Conclusion
The FST Village Playbook ignited the fire needed to mobilize the village, not only to secure the utilities required, but also a bed for Leon to sleep on. In turn, the risk for CPS removal was decreased, and the mother’s depression got remarkably better because she finally had the support that was both clear and measurable with accountability.
Leon, in turn, started performing well in school and attending his juvenile probation community service obligations. Without the extended family and the playbook, it is unlikely that Leon’s family would get unstuck and move forward.
About the author
Scott P. Sells, Ph.D., MSW, LCSW, LMFT, is the author of three books, Treating the Tough Adolescent: A Family-Based, Step-by-Step Guide (1998), Parenting Your Out-of-Control Teenager: 7 Steps to Reestablish Authority and Reclaim Love (2001), and Treating the Traumatized Child: A Step-by-Step Family Systems Approach (2017). He can be contacted at spsells@familytrauma.com or through LinkedIn and Facebook.


One other issue is that if you are in a circumstances where you don’t have a co-signer then you may want to try to make use of all of your federal funding options. You can get many awards and other scholarships or grants that will give you money to help you with institution expenses. Thanks a lot for the post.
Thanks for sharing. I read many of your blog posts, cool, your blog is very good.
S666vegas gives you that Vegas vibe from your phone lol. If you like the Vegas games, its worth looking at to see if it can quench your gambling thirst. Check out the Vegas action here: s666vegas
Hey guys! Jili17login is where it’s at. Super easy to use, and I’ve been having some seriously good luck there. Definitely worth checking out! Go give jili17login a shot, you won’t regret it!
Okbetphp, y’all! This site has been my go-to lately. The odds are pretty sweet, and the interface is smooth as butter. If you’re looking for a new place to bet, check out okbetphp. You might just get lucky!
Your article helped me a lot, is there any more related content? Thanks!
Your point of view caught my eye and was very interesting. Thanks. I have a question for you. https://accounts.binance.info/sl/register-person?ref=I3OM7SCZ
Your point of view caught my eye and was very interesting. Thanks. I have a question for you. https://accounts.binance.com/zh-TC/register?ref=DCKLL1YD
**mitolyn reviews**
Mitolyn is a carefully developed, plant-based formula created to help support metabolic efficiency and encourage healthy, lasting weight management.
Thanks for sharing. I read many of your blog posts, cool, your blog is very good. https://www.binance.com/tr/register?ref=MST5ZREF
**prostafense reviews**
ProstAfense is a premium, doctor-crafted supplement formulated to maintain optimal prostate function, enhance urinary performance, and support overall male wellness.
Your article helped me a lot, is there any more related content? Thanks!
Thanks for sharing. I read many of your blog posts, cool, your blog is very good.
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
Thanks for sharing. I read many of your blog posts, cool, your blog is very good. https://accounts.binance.com/register-person?ref=IXBIAFVY
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
Thanks for sharing. I read many of your blog posts, cool, your blog is very good.
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
Your article helped me a lot, is there any more related content? Thanks! https://accounts.binance.info/fr/register?ref=T7KCZASX
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me. https://www.binance.info/register?ref=IXBIAFVY
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
Buy Ativan Online
**prostafense**
ProstAfense is a premium, doctor-crafted supplement formulated to maintain optimal prostate function, enhance urinary performance, and support overall male wellness.
**prodentim**
ProDentim is a distinctive oral-care formula that pairs targeted probiotics with plant-based ingredients to encourage strong teeth, comfortable gums, and reliably fresh breath.
**nervecalm**
NerveCalm is a high-quality nutritional supplement crafted to promote nerve wellness, ease chronic discomfort, and boost everyday vitality.
**neurosharp**
Neuro Sharp is a modern brain-support supplement created to help you think clearly, stay focused, and feel mentally confident throughout the day.
рейтинг digital агентств [url=https://luchshie-digital-agencstva.ru/]рейтинг digital агентств[/url] .
Статьи о маркетинге https://reklamspilka.org.ua PR и рекламе для бизнеса и специалистов. Практические рекомендации по продвижению брендов, управлению репутацией, контент-стратегии, рекламе в интернете и эффективным коммуникациям с клиентами.
Your article helped me a lot, is there any more related content? Thanks! https://www.binance.com/bn/register?ref=WTOZ531Y
**purdentix**
PurDentix is a revolutionary oral health supplement designed to support strong teeth and healthy gums. It tackles a wide range of dental concerns
**citrusburn**
CitrusBurn is a Mediterranean-inspired thermogenic formula created to support a naturally slower metabolism, encourage efficient fat utilization.
internet seo [url=https://prodvizhenie-sajtov-v-moskve15.ru/]prodvizhenie-sajtov-v-moskve15.ru[/url] .
**prostapeak**
Prosta Peak is a high-quality prostate wellness supplement formulated with a comprehensive blend of 20+ natural ingredients and essential nutrients to support prostate health
**manergy**
Manergy is an advanced male vitality supplement created to help support healthy testosterone levels
**nervegenics**
NerveGenics is a naturally formulated nerve-health supplement created to promote nerve comfort, cellular energy support, antioxidant defense
аудит продвижения сайта prodvizhenie-sajtov-v-moskve15.ru .
Очень понравилось отношение к клиенту — доброжелательно и честно.
букет цветов томск
ProDentim is a distinctive oral-care formula that pairs targeted probiotics with plant-based ingredients to encourage strong teeth, comfortable gums, and reliably fresh breath.
Mitolyn is a carefully developed, plant-based formula created to help support metabolic efficiency and encourage healthy, lasting weight management.
AquaSculpt is a high-quality metabolic support supplement created to help the body utilize fat more efficiently while maintaining steady, reliable energy levels throughout the day.
PurDentix is a revolutionary oral health supplement designed to support strong teeth and healthy gums. It tackles a wide range of dental concerns
Backbiome is a naturally crafted, research-backed daily supplement formulated to gently relieve back tension and soothe sciatic discomfort.
HeroUP is a premium mens wellness formula designed to support sustained energy, physical stamina, and everyday confidence.
Boostaro is a purpose-built wellness formula created for men who want to strengthen vitality, confidence, and everyday performance.
InsuLeaf is a high-quality, naturally formulated supplement created to help maintain balanced blood glucose, support metabolic health, and boost overall vitality.
Maintaining prostate health is crucial for men’s overall wellness, especially as they grow older. Conditions like reduced urine flow, interrupted sleep
The bodys natural process of skin cell renewal is essential for preserving a smooth, healthy, and youthful-looking complexion.
Manergy is an advanced male vitality supplement created to help support healthy testosterone levels
Arialief is a carefully developed dietary supplement designed to naturally support individuals dealing with sciatic nerve discomfort while promoting overall nerve wellness.
NativeGut is a precision-crafted nutritional blend designed to nurture your dog’s digestive tract.
Gluco6 is a natural, plant-based supplement designed to help maintain healthy blood sugar levels.
Kerassentials is an entirely natural blend crafted with 4 potent core oils and enriched by 9 complementary oils and vital minerals.
NerveGenics is a naturally formulated nerve-health supplement created to promote nerve comfort, cellular energy support, antioxidant defense
ProstAfense is a premium, doctor-crafted supplement formulated to maintain optimal prostate function, enhance urinary performance, and support overall male wellness.
Nitric Boost Ultra is a daily wellness formula designed to enhance vitality and help support all-around performance.
GL Pro is a natural dietary supplement formulated to help maintain steady, healthy blood sugar levels while easing persistent sugar cravings.
NerveCalm is a high-quality nutritional supplement crafted to promote nerve wellness, ease chronic discomfort, and boost everyday vitality.
Prostadine concerns can disrupt everyday rhythm with steady discomfort, fueling frustration and a constant hunt for dependable relief.
Prosta Peak is a high-quality prostate wellness supplement formulated with a comprehensive blend of 20+ natural ingredients and essential nutrients to support prostate health
MounjaBoost is a next-generation, plant-based supplement created to support metabolic activity, encourage natural fat utilization
ViriFlow is a dietary supplement formulated to help maintain prostate, bladder, and male reproductive health. Its blend of plant-based ingredients is designed to support urinary comfort and overall wellness as men age.
Visium Pro is an advanced vision support formula created to help maintain eye health, sharpen visual performance, and provide daily support against modern challenges such as screen exposure and visual fatigue.
1xbet tr giri? [url=https://1xbet-51.com/]1xbet tr giri?[/url] .
看不懂但大受震撼
AquaSculpt is a high-quality metabolic support supplement created to help the body utilize fat more efficiently while maintaining steady, reliable energy levels throughout the day.
Prosta Peak is a high-quality prostate wellness supplement formulated with a comprehensive blend of 20+ natural ingredients and essential nutrients to support prostate health
GL Pro is a natural dietary supplement formulated to help maintain steady, healthy blood sugar levels while easing persistent sugar cravings.
NativeGut is a precision-crafted nutritional blend designed to nurture your dog’s digestive tract.
The bodys natural process of skin cell renewal is essential for preserving a smooth, healthy, and youthful-looking complexion.
Backbiome is a naturally crafted, research-backed daily supplement formulated to gently relieve back tension and soothe sciatic discomfort.
MounjaBoost is a next-generation, plant-based supplement created to support metabolic activity, encourage natural fat utilization
1 xbet giri? [url=https://1xbet-giris-31.com/]1 xbet giri?[/url] .
This article feels both timely and insightful, which is a combination I always appreciate. Happy you wrote it, and thankful you shared it here.
Very good i like it
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
Your article helped me a lot, is there any more related content? Thanks! https://www.binance.info/register?ref=IXBIAFVY
VPS server
VPS server-Hosting
Amsterdam
Thanks for sharing. I read many of your blog posts, cool, your blog is very good. https://www.binance.com/register?ref=JW3W4Y3A
Заказать Haval – только у нас вы найдете цены ниже рынка. Быстрей всего сделать заказ на купить новый haval можно только у нас!
[url=https://havalpromsk11.ru]haval купить новый у официального дилера[/url]
haval модели 2025 года – [url=http://www.havalpromsk11.ru/]http://havalpromsk11.ru[/url]
방콕물집
Профессиональная: оклейка авто пленкой в Москве – сохраните родное лакокрасочное покрытие в идеальном состоянии на долгие годы.
대전출장안마
Thank you for your sharing. I am worried that I lack creative ideas. It is your article that makes me full of hope. Thank you. But, I have a question, can you help me?
청주출장마사지
how to get prednisone without a prescription: generic prednisone tablets – prednisone price south africa
wish you all the best
d2qxhu
can i purchase prednisone without a prescription: corticosteroid medication online – prednisone without prescription.net
dog medicine: discount pet meds – dog prescriptions online
http://pawtrustmeds.com/# п»їdog medication online
indian pharmacy online: cheapest online pharmacy india – indian pharmacy
pharmacy website india: legitimate online pharmacies india – india pharmacy
top online pharmacy india: reputable indian online pharmacy – mail order pharmacy india
reddit canadian pharmacy: NorthAccess Rx – canadian pharmacy cheap
http://northaccessrx.com/# www canadianonlinepharmacy
https://globalindiapharmacy.com/# Global India Pharmacy
canadian drug prices: drugs from canada – canadian drug pharmacy
Global India Pharmacy: п»їlegitimate online pharmacies india – Global India Pharmacy
http://pawtrustmeds.com/# Paw Trust Meds
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
Paw Trust Meds: pet pharmacy online – Paw Trust Meds
canada pharmacy world: NorthAccess Rx – best canadian online pharmacy
AquaSculpt is a high-quality metabolic support supplement created to help the body utilize fat more efficiently while maintaining steady
Backbiome is an advanced daily wellness supplement formulated to help support spinal comfort, reduce feelings of built-up tension, and promote freer, smoother movement throughout everyday life.
PurDentix is a revolutionary oral health supplement designed to support strong teeth and healthy gums. It tackles a wide range of dental concerns, including gum inflammation and tooth decay
GL Pro is a natural dietary supplement formulated to help maintain steady, healthy blood sugar levels while easing persistent sugar cravings.
Boostaro is a modern mens wellness formula created to support daily vitality, stamina, and confidence through a practical, natural routine.
NerveCalm is a high-quality nutritional supplement crafted to promote nerve wellness, ease chronic discomfort, and boost everyday vitality.
best online canadian pharmacy: NorthAccess Rx – my canadian pharmacy reviews
https://pawtrustmeds.com/# Paw Trust Meds
https://pawtrustmeds.shop/# Paw Trust Meds
canadian pharmacy in canada: NorthAccess Rx – safe canadian pharmacy
Paw Trust Meds: vet pharmacy – Paw Trust Meds
Global India Pharmacy: cheapest online pharmacy india – Global India Pharmacy
canadian pharmacy: trustworthy canadian pharmacy – best online canadian pharmacy
escrow pharmacy canada: NorthAccess Rx – canadian pharmacy online reviews
https://globalindiapharmacy.com/# world pharmacy india
Global India Pharmacy: Global India Pharmacy – Global India Pharmacy
https://globalindiapharmacy.shop/# reputable indian pharmacies
canadian pharmacy online store: NorthAccess Rx – canadian pharmacy antibiotics
indianpharmacy com: Global India Pharmacy – Global India Pharmacy
https://globalindiapharmacy.com/# india pharmacy
canada drugs online reviews: NorthAccess Rx – canadianpharmacymeds
recommended canadian pharmacies: NorthAccess Rx – canadian pharmacy world
http://northaccessrx.com/# canadian pharmacies
pet meds for dogs: Paw Trust Meds – dog prescriptions online
Global India Pharmacy: Online medicine home delivery – Global India Pharmacy
шумоизоляция автомобиля цена https://shumoizolyaciya-avtomobilya-cena-1.ru
AquaSculpt is a high-quality metabolic support supplement created to help the body utilize fat more efficiently while maintaining steady
Backbiome is an advanced daily wellness supplement formulated to help support spinal comfort, reduce feelings of built-up tension, and promote freer, smoother movement throughout everyday life.
GL Pro is a natural dietary supplement formulated to help maintain steady, healthy blood sugar levels while easing persistent sugar cravings.
canadian pharmacy: legal canadian pharmacy online – canadian pharmacy cheap
pet prescriptions online: dog prescriptions online – Paw Trust Meds
https://globalindiapharmacy.com/# top 10 pharmacies in india
best online canadian pharmacy: NorthAccess Rx – canadian pharmacy online reviews
canadadrugpharmacy com: NorthAccess Rx – canadianpharmacymeds com
Paw Trust Meds: Paw Trust Meds – Paw Trust Meds
indian pharmacy online: indian pharmacy – Global India Pharmacy
canada online pharmacy: adderall canadian pharmacy – online canadian drugstore
recommended canadian pharmacies: my canadian pharmacy review – canadian valley pharmacy
https://globalindiapharmacy.com/# Global India Pharmacy
best online pharmacy india: indian pharmacies safe – Online medicine home delivery
vet pharmacy: vet pharmacy online – online vet pharmacy
What’s the most common mistake people make when starting out with this?
http://pawtrustmeds.com/# Paw Trust Meds
canadian medications: canadian pharmacy online – best canadian pharmacy to buy from
best canadian pharmacy to buy from: canadian drugstore online – online canadian pharmacy
Paw Trust Meds: pet prescriptions online – online vet pharmacy
CoreBlue Health: viagra without prescription – CoreBlue Health
CoreBlue Health buy Viagra over the counter CoreBlue Health
VeritasCare: Tadalafil price – Buy Tadalafil 20mg
https://corebluehealth.com/# CoreBlue Health
https://civicmeds.shop/# pill pharmacy
canada rx pharmacy: CivicMeds – canadian pharmacy tampa
canadian pharmacies online no prescription pharmacy paypal canada pharmacy coupon
reputable canadian online pharmacy: prescription free canadian pharmacy – reputable indian pharmacies
VeritasCare Cialis 20mg price Cialis over the counter
CoreBlue Health: CoreBlue Health – order viagra
https://corebluehealth.shop/# CoreBlue Health
canadian pharmacy checker: CivicMeds – rx pharmacy online
http://corebluehealth.com/# CoreBlue Health
24 hours pharmacy CivicMeds express pharmacy
canada pharmacy online: CivicMeds – online pharmacy store
Cheap generic Viagra online: Viagra tablet online – Cheap Sildenafil 100mg
http://veritascarepharm.com/# VeritasCare
legitimate online pharmacy usa CivicMeds no rx pharmacy
Buy generic 100mg Viagra online: Order Viagra 50 mg online – CoreBlue Health
best mail order pharmacy canada: pharmacy in canada for viagra – canadian pharmacies compare
CoreBlue Health cheapest viagra Viagra Tablet price
best no prescription pharmacy: CivicMeds – top online pharmacy 247
http://veritascarepharm.com/# VeritasCare
https://civicmeds.shop/# us pharmacy
CoreBlue Health: CoreBlue Health – CoreBlue Health
CoreBlue Health CoreBlue Health CoreBlue Health
reputable canadian online pharmacy: CivicMeds – pharmacy express
pharmacy rx: no rx pharmacy – reputable online pharmacy no prescription
online pharmacy in turkey CivicMeds pharmacy in canada
http://veritascarepharm.com/# VeritasCare
online shopping pharmacy india: legitimate mexican pharmacy online – india pharmacy mail order
trustworthy online pharmacy: CivicMeds – canada drugs online
online pharmacy dubai canadianpharmacyworld pharmacy coupons
http://corebluehealth.com/# Cheapest Sildenafil online
usa pharmacy: CivicMeds – canadian pharmacy phone number
https://corebluehealth.shop/# CoreBlue Health
save on pharmacy: express scripts pharmacy – cheapest pharmacy for prescriptions without insurance
canadian pharmacy sildenafil CivicMeds canadian pharmacy online cialis
rx pharmacy: northwest pharmacy canada – canadian pharmacy prices
VeritasCare: VeritasCare – VeritasCare
Cialis over the counter VeritasCare VeritasCare
https://veritascarepharm.com/# Cialis without a doctor prescription
VeritasCare: Tadalafil Tablet – VeritasCare
Generic Viagra online: sildenafil online – Cheap generic Viagra online
CoreBlue Health cheap viagra Viagra Tablet price
п»їcialis generic: VeritasCare – VeritasCare
https://corebluehealth.com/# Cheap generic Viagra online
Tadalafil price: VeritasCare – VeritasCare
Buy Cialis online Tadalafil Tablet Cialis 20mg price in USA
Thank you for your sharing. I am worried that I lack creative ideas. It is your article that makes me full of hope. Thank you. But, I have a question, can you help me? https://startupfever.de/marc-schammel/?unapproved=18682&moderation-hash=9eef43690182721f2d542b0ce9f805b9#comment-18682
Viagra online price: Generic Viagra online – buy viagra here
https://veritascarepharm.com/# VeritasCare
Generic Cialis price Tadalafil price Generic Cialis price
mail order pharmacy india: canada pharmacy online legit – canadian pharmacy no scripts
https://civicmeds.com/# family pharmacy
polish pharmacy online uk: CivicMeds – mexican pharmacy online
CoreBlue Health CoreBlue Health Generic Viagra online
Cialis over the counter: Cialis 20mg price – VeritasCare
Buy Tadalafil 20mg: п»їcialis generic – Buy Tadalafil 10mg
https://veritascarepharm.shop/# buy cialis pill
https://civicmeds.shop/# online pharmacy price checker
on line pharmacy on line pharmacy super pharmacy
VeritasCare: Tadalafil Tablet – cialis for sale
CoreBlue Health: CoreBlue Health – CoreBlue Health
pharmacy wholesalers canada rx pharmacy online 24 top 10 online pharmacy in india
Cialis without a doctor prescription: Buy Tadalafil 10mg – VeritasCare
http://veritascarepharm.com/# VeritasCare
mexican pharmacy online: CivicMeds – your pharmacy online
VeritasCare Cialis without a doctor prescription Tadalafil Tablet
buy cialis pill: cialis for sale – Tadalafil Tablet
https://veritascarepharm.com/# VeritasCare
Your article helped me a lot, is there any more related content? Thanks!
Cheap Cialis: VeritasCare – VeritasCare
CoreBlue Health CoreBlue Health CoreBlue Health
Cialis without a doctor prescription: VeritasCare – VeritasCare
canadian discount pharmacy: professional pharmacy – pharmacy rx
CoreBlue Health: buy Viagra over the counter – Cheap Viagra 100mg
http://civicmeds.com/# escrow pharmacy canada
online pharmacy pain: CivicMeds – canadian pharmacy in canada
Generic Cialis price VeritasCare Tadalafil price
VeritasCare: Buy Tadalafil 10mg – VeritasCare
CoreBlue Health: CoreBlue Health – generic sildenafil
canadian pharmacy generic viagra CivicMeds online pharmacy discount code
VeritasCare: VeritasCare – Generic Cialis without a doctor prescription
CoreBlue Health: Sildenafil Citrate Tablets 100mg – Cheap generic Viagra online
cheap viagra online canadian pharmacy canadian drug pharmacy canada pharmacy coupon
VeritasCare: Buy Tadalafil 10mg – VeritasCare
https://civicmeds.shop/# online pharmacy without insurance
best rogue online pharmacy: cheapest pharmacy for prescription drugs – legal online pharmacies in the us
canada drugs reviews legal online pharmacy california pharmacy
VeritasCare: VeritasCare – Buy Tadalafil 20mg
Tadalafil Tablet VeritasCare Buy Tadalafil 5mg
https://veritascarepharm.shop/# VeritasCare
online pharmacy ordering tops pharmacy canadianpharmacyworld
http://veritascarepharm.com/# cialis for sale
VeritasCare buy cialis pill Cialis 20mg price
order viagra sildenafil online order viagra
https://veritascarepharm.com/# VeritasCare
sildenafil online CoreBlue Health Viagra Tablet price
https://corebluehealth.shop/# Cheap Sildenafil 100mg
https://corebluehealth.com/# CoreBlue Health
on line pharmacy CivicMeds script pharmacy
Cialis over the counter VeritasCare Generic Cialis price
http://civicmeds.com/# legitimate canadian pharmacy online
CoreBlue Health CoreBlue Health sildenafil over the counter
Tadalafil Tablet Buy Tadalafil 5mg VeritasCare
https://corebluehealth.shop/# CoreBlue Health
http://civicmeds.com/# vipps canadian pharmacy
Cialis without a doctor prescription: cheapest cialis – п»їcialis generic
sure save pharmacy world pharmacy india best european online pharmacy
http://veritascarepharm.com/# cialis generic
generic sildenafil: CoreBlue Health – CoreBlue Health
CoreBlue Health CoreBlue Health Order Viagra 50 mg online
online otc pharmacy: CivicMeds – cheapest prescription pharmacy
24 hours pharmacy CivicMeds online pharmacy china
http://veritascarepharm.com/# Generic Tadalafil 20mg price
Cialis without a doctor prescription: Buy Tadalafil 5mg – VeritasCare
Buy Tadalafil 20mg cialis for sale Buy Cialis online
https://civicmeds.shop/# canadian mail order pharmacy
VeritasCare: VeritasCare – Buy Cialis online
VeritasCare VeritasCare п»їcialis generic
http://veritascarepharm.com/# VeritasCare
canadian 24 hour pharmacy: list of online pharmacies – escrow pharmacy online
VeritasCare Buy Tadalafil 5mg Cheap Cialis
https://civicmeds.shop/# online pharmacy price checker
Generic Viagra for sale: Sildenafil Citrate Tablets 100mg – CoreBlue Health
VeritasCare Cialis without a doctor prescription Cialis 20mg price in USA
https://veritascarepharm.com/# VeritasCare
cheapest viagra: CoreBlue Health – CoreBlue Health
Viagra without a doctor prescription Canada CoreBlue Health CoreBlue Health
https://corebluehealth.shop/# CoreBlue Health
https://pinupazz.top/ pin up casino
https://pinupazz.top/ pin up casino
пин ап пин ап кз
pin up pin-up oyunu
pin up pin-up online casino
https://pinupaz.online/ pin-up oyunu
https://pin-up-kz.space/ пин ап казахстан
pin up pin up
Your article helped me a lot, is there any more related content? Thanks!
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
https://pinupaz.online/ pin up
https://pin-up-kz.space/ пин ап казахстан
pin up pin up casino
https://pinupaz.online/ pin-up online casino
https://pinupazz.top/ pin up az
https://pin-up-kz.space/ пин ап кз
pin up pin up
https://pin-up-kz.space/ пин ап казино kz
https://pinupazz.top/ pin up az
pin up pin up
пин ап пин ап казахстан
https://pinupaz.online/ pin up casino
https://pin-up-kz.space/ пин ап казахстан
pin up pin-up oyunu
https://pinupazz.top/ pin-up oyunu
https://pin-up-kz.space/ пин ап казахстан
trustworthy online pharmacy: online pharmacy india – п»їinternational drug mart
online pharmacy without prescription: india pharmacy – legit online pharmacy
https://formulinepharmacy.shop/# pharmacy websites
reputable overseas online pharmacies: cheapest online pharmacy india – safe online pharmacies
AccessBridge: mexican pharma – AccessBridge
https://formulinepharmacy.shop/# pharmacy online
global pharmacy canada canadian pharmacy in canada SteadyMeds pharmacy
SteadyMeds: SteadyMeds pharmacy – SteadyMeds pharmacy
https://formulinepharmacy.shop/# no rx needed pharmacy
online pharmacies: FormuLine Pharmacy – top online pharmacy
best canadian online pharmacy reviews: SteadyMeds pharmacy – canadian pharmacy review
https://accessbridgepharmacy.shop/# AccessBridge Pharmacy
SteadyMeds: canadian pharmacy oxycodone – SteadyMeds
AccessBridge Pharmacy: AccessBridge Pharmacy – AccessBridge Pharmacy
SteadyMeds SteadyMeds pharmacy SteadyMeds pharmacy
https://formulinepharmacy.com/# worldwide pharmacy online
best online pharmacy: buy prescription drugs from india – top online pharmacy
AccessBridge Pharmacy: is mexipharmacy legit – best mexican pharmacy
http://steadymedspharmacy.com/# SteadyMeds
northwest canadian pharmacy: canadian online drugstore – canadian drugs online
https://accessbridgepharmacy.shop/# mexico online farmacia
http://steadymedspharmacy.com/# reputable canadian pharmacy
top-rated online pharmacies: top 10 online pharmacy in india – top online pharmacy
online pharmacy discount code FormuLine Pharmacy pharmacy order online
https://steadymedspharmacy.shop/# SteadyMeds pharmacy
http://accessbridgepharmacy.com/# AccessBridge Pharmacy
legal online pharmacy: reputable indian pharmacies – legitimate online pharmacy
best rx pharmacy online: indianpharmacy com – online pharmacy discount code
http://formulinepharmacy.com/# medicine online
legitimate online pharmacy: best online pharmacy india – online pharmacies
canadian pharmacy 365 SteadyMeds pharmacy SteadyMeds pharmacy
http://formulinepharmacy.com/# pharmacy websites
https://formulinepharmacy.com/# online pharmacy no prescription needed
precription drugs from canada: best rated canadian pharmacy – SteadyMeds
https://formulinepharmacy.shop/# worldwide pharmacy
https://formulinepharmacy.com/# international pharmacy
AccessBridge: AccessBridge Pharmacy – purple pharmacy online
pharmacy canadian: SteadyMeds pharmacy – SteadyMeds
los algodones pharmacy online mexi pharmacy AccessBridge
https://accessbridgepharmacy.shop/# AccessBridge
pharmacy in mexico online: AccessBridge Pharmacy – AccessBridge
https://accessbridgepharmacy.shop/# mexican medicine store
http://formulinepharmacy.com/# online pharmacy discount code
SteadyMeds: canadian pharmacy – SteadyMeds pharmacy
AccessBridge Pharmacy: AccessBridge – AccessBridge Pharmacy
https://steadymedspharmacy.shop/# SteadyMeds pharmacy
escrow pharmacy canada canadian pharmacies comparison safe canadian pharmacies
worldwide pharmacy online: FormuLine Pharmacy – international pharmacy
http://accessbridgepharmacy.com/# AccessBridge Pharmacy
http://steadymedspharmacy.com/# SteadyMeds
reputable overseas online pharmacies: india pharmacy mail order – no prescription pharmacy paypal
https://formulinepharmacy.com/# pharmacy websites
http://steadymedspharmacy.com/# SteadyMeds
AccessBridge Pharmacy: progreso, mexico pharmacy online – AccessBridge Pharmacy
SteadyMeds: SteadyMeds – SteadyMeds
foreign online pharmacy buy medicines online in india worldwide pharmacy
https://accessbridgepharmacy.com/# AccessBridge Pharmacy
reputable canadian online pharmacy: SteadyMeds pharmacy – SteadyMeds pharmacy
http://steadymedspharmacy.com/# SteadyMeds pharmacy
best mail order pharmacy: indian pharmacy paypal – best mail order pharmacy
https://formulinepharmacy.com/# online pharmacy no rx
mexican pharmacy menu: purple pharmacy – online pharmacy
https://formulinepharmacy.com/# legit online pharmacy
방콕유흥
the canadian pharmacy: best canadian pharmacy to order from – SteadyMeds pharmacy
mexico medicine AccessBridge AccessBridge Pharmacy
https://steadymedspharmacy.shop/# canadian pharmacies comparison
SteadyMeds pharmacy: legit canadian pharmacy online – SteadyMeds pharmacy
canada discount pharmacy: SteadyMeds – SteadyMeds
https://formulinepharmacy.shop/# best mail order pharmacy
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me. https://accounts.binance.info/id/register-person?ref=UM6SMJM3
canadian pharmacy scam: SteadyMeds – SteadyMeds
AccessBridge: purple pharmacy mexico – mexican pharmacies that ship to us
http://accessbridgepharmacy.com/# AccessBridge
mexican drugstore pharmacies in mexico progreso mexico pharmacy online
https://accessbridgepharmacy.com/# purple pharmacy
SteadyMeds: SteadyMeds – SteadyMeds pharmacy
onlinecanadianpharmacy: SteadyMeds – SteadyMeds
https://steadymedspharmacy.shop/# canadian pharmacies compare
online pharmacy without prescription FormuLine Pharmacy reputable overseas online pharmacies
AccessBridge Pharmacy: AccessBridge Pharmacy – AccessBridge
mexican drug stores: mexican pharmacy that ships to the us – meds from mexico
If you want to browse a notes-style resource in the gambling niche https://plicpad.com with a smooth browsing experience designed for regular users can serve as a practical option to compare when you want a site with a practical and modern structure by combining clarity, variety, ease of use, effective organization, well-distributed content, intuitive access and practical reading comfort.
Pet Canada Direct: Pet Canada Direct – canada pet meds
https://edmedscoupon.shop/# online erectile dysfunction medication
cheap ed medicine: Ed Meds Coupon – trusted online pharmacy
where to get ed pills: where can i get ed pills – online drugs order
Pet Canada Direct Pet Canada Direct Pet Canada Direct
http://petcanadadirect.com/# online pet pharmacy
reliable online pharmacy: Pharm Rate – Pharm Rate
http://petcanadadirect.com/# Pet Canada Direct
online pharmacies: online drugs order – legal online pharmacies in the us
ed rx online: ed online pharmacy – online pharmacy no rx
Pharm Rate Pharm Rate pharmacy online
http://edmedscoupon.com/# ed medicine online
cheapest ed medication: Ed Meds Coupon – new pharmacy online
ed meds cheap: Ed Meds Coupon – pharmacy order online
https://petcanadadirect.com/# vet pharmacy
Pet Canada Direct: vet pharmacy – pet pharmacy
medicine online Pharm Rate Pharm Rate
Pet Canada Direct: Pet Canada Direct – pet meds official website
https://edmedscoupon.com/# ed treatment online
Pet Canada Direct: Pet Canada Direct – Pet Canada Direct
vfWVKBrzgUUGcyDpf
https://petcanadadirect.com/# Pet Canada Direct
Pharm Rate international pharmacy Pharm Rate
ed medicine online: Ed Meds Coupon – pharmacy websites
Pet Canada Direct: Pet Canada Direct – dog medicine
https://pharmrate.com/# Pharm Rate
pet meds for dogs: pet pharmacy online – online pet pharmacy
Pet Canada Direct: best pet rx – discount pet meds
https://pharmrate.com/# best online pharmacy
Pharm Rate: Pharm Rate – best rx pharmacy online
Pharm Rate online pharmacy discount code no script pharmacy
get antibiotics without seeing a doctor: prescription antibiotic – antibiotics cheap
https://stromectol.reviews/# stromectol australia
semaglutide thyroid: semaglutide life – medicine online
buy stromectol canada: ivermectin – ivermectin price usa
https://semaglutide.life/# is zepbound a semaglutide
YtJyIFfSFQdpySKB
ivermectin over the counter stromectol oral where to buy ivermectin
stromectol reviews: stromectol reviews – stromectol reviews
over the counter antibiotics: over the counter antibiotics – over the counter antibiotics
https://semaglutide.life/# can you take rybelsus and mounjaro together
over the counter antibiotics: over the counter antibiotics – antibiotics cheap
https://semaglutide.life/# rybelsus glp-1
stromectol reviews ivermectin 18mg buy stromectol
ivermectin generic: ivermectin 4 – stromectol 6 mg tablet
can you take 2 3 mg rybelsus: semaglutide life – top online pharmacy
https://stromectol.reviews/# stromectol reviews
over the counter antibiotics: over the counter antibiotics – over the counter antibiotics
stromectol reviews: stromectol prices – stromectol reviews
https://stromectol.reviews/# buy ivermectin pills
stromectol reviews stromectol reviews stromectol reviews
stromectol liquid: ivermectin for humans – stromectol buy
Промокод при регистрации 1xbet на 32 500 рублей. Этот код нужно ввести при регистрации в соответствующее поле. 1Xbet промокод можно использовать только один раз, но им можно делиться с друзьями. Регистрация по номеру телефона — быстрый способ создать аккаунт. После получения данных для входа остаётся лишь ввести логин и пароль. Используй актуальный промокод 1хбет при регистрации и увеличь первый депозит до 32 500 рублей в БК 1xBet. На платформе действует система вознаграждений, которая помогает игрокам получать до дополнительных процентов от первого депозита.
https://antibiotics.cheap/# antibiotics cheap
antibiotics cheap: cheap antibiotics – over the counter antibiotics
buy antibiotics online for tooth infection: antibiotics cheap – buy antibiotics online
https://semaglutide.life/# semaglutide alternatives
Pokies Australia has so much to offer when it comes to variety. I’ve been trying to find the [url=https://au-online-pokies.com/]https://au-online-pokies.com/[/url] for a while now. Is it just me, or do some sites really have better graphics and themes than others? I’m always impressed by how creative these developers can get. Would love to hear your thoughts on which games have caught your eye!
rybelsus vs farxiga: semaglutide life – buy online medicine
stromectol how much it cost stromectol reviews generic ivermectin cream
antibiotic without presription: buy antibiotics over the counter – over the counter antibiotics
Контент завод представляет собой эффективный механизм создания уникального контента.
Если вы хотите быстро и эффективно создать уникальные материалы для своего проекта, обязательно посетите [url=https://sitehui.ru]контент завод н8н[/url].
Клиенты имеют возможность подобрать стиль, тематику и объем материалов под свои нужды.
https://semaglutide.life/# semaglutide for alcoholism
over the counter antibiotics: buy zithromax antibiotic – antibiotics cheap
semaglutide storage: semaglutide life – online pharmacy without prescription
https://antibiotics.cheap/# generic antibiotics online cheap
order stromectol: stromectol 3 mg tablet – stromectol reviews
how long for rybelsus to leave your system semaglutide life rybelsus tab 14mg
rybelsus stomach pain: rybelsus a1c reduction – reputable online pharmacy no prescription
https://shorturl.fm/DKTzY
https://stromectol.reviews/# stromectol reviews
can you take semaglutide with high blood pressure medication: semaglutide life – online pharmacy no rx
buy stromectol online uk: cost of ivermectin 1% cream – stromectol 3 mg dosage
https://semaglutide.life/# rybelsus and coffee
otc medicine: over the counter antibiotics – antibiotics cheap
ozempic o rybelsus para adelgazar does rybelsus cause weight loss ro semaglutide
over the counter antibiotics: antibiotics cheap – get antibiotics quickly
https://antibiotics.cheap/# antibiotics cheap
antibiotics cheap: over the counter antibiotics – over the counter antibiotics
antibiotics for uti over the counter: antibiotics cheap – prescribed antibiotics online
https://antibiotics.cheap/# over the counter antibiotics
Over the counter antibiotics pills: antibiotics cheap – generic antibiotics online cheap
stromectol reviews stromectol reviews stromectol reviews
over the counter antibiotics: antibiotics cheap – antibiotics cheap
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article. https://accounts.binance.info/register-person?ref=IXBIAFVY
https://antibiotics.cheap/# cheap antibiotics
antibiotics cheap: over the counter antibiotics – over the counter antibiotics
prescription antibiotic: over the counter antibiotics – over the counter antibiotics
https://semaglutide.life/# semaglutide atlanta
semaglutide otc: semaglutide skin sensitivity – worldwide pharmacy
is zepbound semaglutide: how much does rybelsus lower a1c – reputable overseas online pharmacies
ivermectin 90 mg ivermectin oral 0 8 stromectol reviews
https://semaglutide.life/# semaglutide cost per month
ivermectin: stromectol reviews – stromectol covid
stromectol reviews: stromectol reviews – stromectol reviews
https://semaglutide.life/# does rybelsus cause kidney problems
long term effects of semaglutide: where can i get semaglutide for weight loss – us pharmacy no prescription
buy amoxicillin: over the counter antibiotics – get antibiotics quickly
https://antibiotics.cheap/# over the counter antibiotics
alcohol and semaglutide how long does semaglutide last in fridge when to take rybelsus
semaglutide refrigeration: semaglutide life – safe online pharmacies
stromectol reviews: stromectol reviews – stromectol reviews
https://antibiotics.cheap/# antibiotics cheap
antibiotics cheap: buy antibiotics for sinus – buy antibiotics for uti
Market analysts confirm as if acquiring off-plan apartments during long-term investment gives the opportunity families not only get a 10-year Golden Visa, as well as smoothly strengthen personal financial potential in the context of booming tourism.
Website https://buy-property-uae.com/
https://semaglutide.life/# do you lose weight on rybelsus
weight watchers semaglutide reviews semaglutide life online semaglutide gomedidirect.com
what happens if you take rybelsus with food: low cost semaglutide – foreign online pharmacy
semaglutide san antonio: 0.25 semaglutide – shop medicine online
https://semaglutide.life/# semaglutide sublingual dose
rybelsus side effects 3 mg: semaglutide life – no script pharmacy
generic antibiotics: antibiotics cheap – antibiotics drugs
http://mexicanpharm.com/# Mexican Pharm
pharmacies in canada that ship to the us Canadian Tabs canadian drug
legitimate canadian pharmacy: Canadian Tabs – canada drugs
pharmacy website india: india pharmacy mail order – no rx needed pharmacy
https://mexicanpharm.xyz/# mexico pharmacy price list
Mexican Pharm: Mexican Pharm – п»їmexican pharmacy
order meds from mexico: mexican pharmacy that ships to the us – Mexican Pharm
https://indianmedsdelivery.xyz/# india online pharmacy
legitimate canadian pharmacy Canadian Tabs Canadian Tabs
Canadian Tabs: buying from canadian pharmacies – Canadian Tabs
Canadian Tabs: Canadian Tabs – Canadian Tabs
https://indianmedsdelivery.com/# online pharmacy india
world pharmacy india: cheapest online pharmacy india – best online pharmacy no prescription
Если хотите apple macbook air m4 купить[/url], заходите на наш сайт!
При выборе модели обратите внимание на диагональ экрана и вес, особенно если вы часто берёте ноутбук с собой.
Mexican Pharm: Mexican Pharm – Mexican Pharm
http://indianmedsdelivery.com/# mail order pharmacy india
best online pharmacy india Indian Meds Delivery online pharmacy no prescription
mexican mail order pharmacy: pharmacy mexico – pharmacies in mexico that ship to the us
https://mexicanpharm.com/# Mexican Pharm
cheapest online pharmacy india: buy medicines online in india – medstore online pharmacy
Mexican Pharm: pharmacy delivery – Mexican Pharm
http://canadiantabs.com/# Canadian Tabs
pharmacys in mexico: Mexican Pharm – mexico online pharmacy
ordering drugs from canada: canadian drugs online – Canadian Tabs
mexican pharmacy online medications Mexican Pharm Mexican Pharm
https://mexicanpharm.com/# the purple pharmacy mexico
mexicanrxpharm: Mexican Pharm – Mexican Pharm
northwest canadian pharmacy: canadianpharmacyworld – canada rx pharmacy world
http://canadiantabs.com/# canadian pharmacy mall
world pharmacy india: reputable indian online pharmacy – pharmacy websites
canada online pharmacy: Canadian Tabs – vipps canadian pharmacy
Canadian Tabs Canadian Tabs Canadian Tabs
https://mexicanpharm.com/# Mexican Pharm
Mexican Pharm: mexico pharmacy online – Mexican Pharm
canadian pharmacy antibiotics: Canadian Tabs – Canadian Tabs
http://mexicanpharm.com/# my mexican pharmacy
mexican pharmacy what to buy: best mexican online pharmacy – Mexican Pharm
hydrocodone mexico pharmacy: legitimate mexican pharmacy online – mexican drugstore
Canadian Tabs Canadian Tabs canadian pharmacy world reviews
https://canadiantabs.com/# Canadian Tabs
my canadian pharmacy rx: drugs from canada – canadian pharmacy world reviews
purple pharmacy: mexican pharmacy online – Mexican Pharm
https://vetpharmfirst.com/# dog prescriptions online
dog prescriptions online: Vet Pharm First – Vet Pharm First
medicine online: Online Pharm First – express scripts mail order pharmacy
Vet Pharm First pet meds official website canada pet meds
https://onlinepharmfirst.shop/# pharmacy websites
pharmacy no prescription required: Online Pharm First – no prescription pharmacy paypal
pet meds for dogs: Vet Pharm First – Vet Pharm First
https://vetpharmfirst.shop/# pet med
medicine online order: no prescription needed pharmacy – online pharmacy without scripts
vet pharmacy: Vet Pharm First – vet pharmacy
reliable online pharmacy international pharmacy reputable overseas online pharmacies
https://ivermectinfirst.shop/# Ivermectin First
Ivermectin First: purchase stromectol online – Ivermectin First
stromectol tablets: Ivermectin First – stromectol tablet 3 mg
https://onlinepharmfirst.com/# best online pharmacy no prescription
ivermectin tablets: Ivermectin First – cost of ivermectin
top online pharmacy: Online Pharm First – buy drugs online
Ivermectin First Ivermectin First stromectol where to buy
http://onlinepharmfirst.com/# shop medicine online
stromectol usa: ivermectin 12 mg – stromectol 3 mg price
http://vetpharmfirst.com/# Vet Pharm First
Ivermectin First: Ivermectin First – ivermectin 2%
stromectol in canada: stromectol pill – Ivermectin First
https://ivermectinfirst.com/# ivermectin australia
online pet pharmacy: pet pharmacy online – pet meds for dogs
замена венцов новокузнецк
no script pharmacy Online Pharm First no rx needed pharmacy
amoxicillin pink pill a 66 pet antibiotics amoxicillin [url=https://fforhimsvipp.com/buy-amoxil/]amoxicillin 500 mg[/url] does cefdinir have amoxicillin in it amoxicillin how many mg
https://onlinepharmfirst.shop/# express scripts mail order pharmacy
Vet Pharm First: dog prescriptions online – pet prescriptions online
https://onlinepharmfirst.shop/# overseas pharmacy no prescription
Vet Pharm First: Vet Pharm First – п»їdog medication online
order stromectol: Ivermectin First – Ivermectin First
https://vetpharmfirst.com/# Vet Pharm First
best rx pharmacy online: Online Pharm First – no rx needed pharmacy
Vet Pharm First dog prescriptions online online vet pharmacy
https://ivermectinfirst.shop/# ivermectin price uk
Vet Pharm First: Vet Pharm First – Vet Pharm First
https://vetpharmfirst.com/# Vet Pharm First
best pet rx: dog prescriptions online – Vet Pharm First
https://onlinepharmfirst.shop/# top online pharmacy
dog medicine Vet Pharm First vet pharmacy
Ivermectin First: ivermectin 1 topical cream – ivermectin otc
https://ivermectinfirst.shop/# ivermectin brand
pet med: Vet Pharm First – Vet Pharm First
https://vetpharmfirst.shop/# best pet rx
reputable online pharmacy no prescription: Online Pharm First – best online pharmacy no prescription
pet pharmacy pet meds official website pet rx
https://onlinepharmfirst.shop/# reputable online pharmacy no prescription
pharmacy online: Online Pharm First – online pharmacies
ivermectin cream canada cost: Ivermectin First – Ivermectin First
http://onlinepharmfirst.com/# worldwide pharmacy online
pet meds for dogs: pet meds for dogs – vet pharmacy online
Ivermectin First Ivermectin First Ivermectin First
https://ivermectinfirst.shop/# Ivermectin First
ivermectin 50 mg: Ivermectin First – Ivermectin First
https://rybelsus.pro/# switching from mounjaro to semaglutide
https://cialis.sbs/# Generic Tadalafil 20mg price
how much weight can you lose with semaglutide semaglutide max dose п»їinternational drug mart
https://rybelsus.pro/# rybelsus for diabetes
buy Viagra over the counter buy Viagra over the counter Cheapest Sildenafil online
Buy Tadalafil 10mg Generic Cialis without a doctor prescription Cialis 20mg price
https://rybelsus.pro/# semaglutide online prescription
https://rybelsus.pro/# can you take semaglutide with high blood pressure medication
Generic Viagra for sale Sildenafil Citrate Tablets 100mg sildenafil over the counter
https://viagra.onl/# Cheap Sildenafil 100mg
https://rybelsus.pro/# semaglutide side effects long term
buy Viagra online Cheap generic Viagra online Cheap Sildenafil 100mg
Cheap generic Viagra online Viagra online price Cheap generic Viagra online
https://viagra.onl/# viagra without prescription
https://viagra.onl/# viagra canada
how to inject compounded semaglutide generic semaglutide online pharmacy without scripts
https://rybelsus.pro/# novo nordisk rybelsus coupon
https://cialis.sbs/# Buy Tadalafil 10mg
order semaglutide rybelsus 7mg safe online pharmacies
Cheap generic Viagra online viagra without prescription cheap viagra
https://cialis.sbs/# Cialis 20mg price in USA
Generic Cialis price Cialis 20mg price in USA Cialis over the counter
https://rybelsus.pro/# rybelsus medscape
how to taper off trazodone 100 mg [url=https://trazomed.com/]order trazodone online[/url] how much trazodone for 70 lb dog
how much trazodone for a 20 pound dog https://trazomed.com/ – trazodone cost without insurance
https://viagra.onl/# sildenafil 50 mg price
Viagra Tablet price Buy Viagra online cheap buy viagra here
how many mg is 10 units of semaglutide zepbound vs semaglutide how to take rybelsus 3 mg
https://viagra.onl/# Sildenafil 100mg price
https://cialis.sbs/# Cheap Cialis
buy cialis pill Cialis without a doctor prescription Tadalafil Tablet
https://cialis.sbs/# Cialis 20mg price in USA
https://viagra.onl/# order viagra
generic sildenafil Sildenafil Citrate Tablets 100mg Sildenafil Citrate Tablets 100mg
rybelsus copay card semaglutide stopped working semaglutide (rybelsus)
https://rybelsus.pro/# rybelsus pcos
Cialis without a doctor prescription buy cialis pill Generic Tadalafil 20mg price
https://cialis.sbs/# cheapest cialis
https://cialis.sbs/# Buy Tadalafil 20mg
Cialis over the counter Buy Tadalafil 5mg Buy Cialis online
https://viagra.onl/# buy Viagra over the counter
Buy Cialis online Cialis 20mg price cialis for sale
cialis for sale Tadalafil Tablet Buy Tadalafil 5mg
https://cialis.sbs/# Buy Cialis online
화성출장안마
Does your blog have a contact page? I’m having a tough time locating
it but, I’d like to send you an e-mail. I’ve got some recommendations for your
blog you might be interested in hearing. Either way, great blog and I look forward to seeing
it improve over time.
https://viagra.onl/# Viagra Tablet price
difference between compounded semaglutide and ozempic can you take metformin and rybelsus together best online pharmacy
https://rybelsus.pro/# rybelsus other name
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
п»їcialis generic Buy Tadalafil 5mg Buy Tadalafil 5mg
https://viagra.onl/# Viagra tablet online
https://rybelsus.pro/# rybelsus medication side effects
how much semaglutide should i take how much does rybelsus cost best online pharmacy
https://viagra.onl/# Cheap Viagra 100mg
https://cialis.sbs/# Generic Cialis price
why does rybelsus cause nausea how to speed up weight loss on semaglutide? us pharmacy no prescription
Fantastic site A lot of helpful info here Im sending it to some buddies ans additionally sharing in delicious And naturally thanks on your sweat
https://rybelsus.pro/# rybelsus stock
diabetes medications rybelsus does rybelsus cause depression when is the best time to take semaglutide
https://viagra.onl/# buy Viagra online
pusulabet: pusulabet güncel
https://casivipgiris.site# bahiscasino güncel giriş
pusulabet güncel pusulabet güncel adres
bahiscasino casino: bahiscasino güncel
bahiscasino giris bahiscasino resmi giriş
https://casivipgiris.site# bahiscasino güncel
Cheapest Sildenafil online order viagra order viagra
pusulabet resmi giriş pusulabet resmi giriş
Easy Canada Meds: safe reliable canadian pharmacy – onlinecanadianpharmacy 24
world pharmacy india Easy India Meds overseas pharmacy no prescription
pharmacy in mexico: mexi pharmacy – Easy Mex Meds
legitimate canadian pharmacies my canadian pharmacy reviews canadian pharmacy scam
https://easymexmeds.shop/# Easy Mex Meds
indian pharmacy online: indian pharmacies safe – medicine online
Easy Canada Meds: canada rx pharmacy – Easy Canada Meds
mexico farmacia Easy Mex Meds Easy Mex Meds
Easy Canada Meds: Easy Canada Meds – Easy Canada Meds
vipps approved canadian online pharmacy: canadian pharmacy sarasota – Easy Canada Meds
india pharmacy india pharmacy legit online pharmacy
http://easycanadameds.com/# Easy Canada Meds
Easy Mex Meds: mail order pharmacy mexico – Easy Mex Meds
india online pharmacy: Easy India Meds – best rx pharmacy online
Easy Mex Meds hydrocodone mexico pharmacy mexican meds
Easy Canada Meds: canadian pharmacy 365 – canadian world pharmacy
Easy Mex Meds: Easy Mex Meds – mexican pharmacies online drugs
Easy Mex Meds mexican pharmacies near me Easy Mex Meds
online pharmacy canada: Easy Canada Meds – cheap canadian pharmacy
https://easymexmeds.com/# pharmacys in mexico
Explicit web platform offers a range of videos for adult entertainment.
Select reliable platforms for a safe experience.
online canadian pharmacy reviews: canadian pharmacy 24h com – canadian pharmacy phone number
Easy Mex Meds mexican online mail order pharmacy Easy Mex Meds
buy medicines online in india: top online pharmacy india – legit online pharmacy
п»їlegitimate online pharmacies india online shopping pharmacy india online pharmacies
buy prescription drugs from india: Easy India Meds – legit online pharmacy
Online medicine home delivery: Easy India Meds – worldwide pharmacy online
http://easyindiameds.com/# world pharmacy india
best rated canadian pharmacy Easy Canada Meds Easy Canada Meds
india pharmacy: mail order pharmacy india – online pharmacy no prescription needed
pharmacy website india: online pharmacy india – online pharmacy without scripts
farmacia mexicana online Easy Mex Meds Easy Mex Meds
the purple pharmacy mexico: Easy Mex Meds – mexican mail order pharmacy
is canadian pharmacy legit: Easy Canada Meds – real canadian pharmacy
world pharmacy india Easy India Meds online drugs order
buy medicines online in india: best online pharmacy india – reputable overseas online pharmacies
https://easyindiameds.shop/# reputable indian pharmacies
reputable indian pharmacies world pharmacy india best online pharmacy no prescription
Easy Canada Meds: pharmacy wholesalers canada – Easy Canada Meds
mexican pharmacy that ships to the us: mexican pharmacy online medications – Easy Mex Meds
Easy Canada Meds best online canadian pharmacy Easy Canada Meds
Easy Mex Meds: Easy Mex Meds – farmacia pharmacy mexico
Easy Canada Meds: Easy Canada Meds – escrow pharmacy canada
vipps canadian pharmacy Easy Canada Meds Easy Canada Meds
top online pharmacy india: Easy India Meds – safe online pharmacies
https://easycanadameds.com/# Easy Canada Meds
reputable canadian online pharmacies: Easy Canada Meds – Easy Canada Meds
canadian drug pharmacy canadianpharmacymeds Easy Canada Meds
Amazing! This website is seriously addictive! The selection of
trans porn videos is massive – loads of stunning trans
girls in crystal-clear scenes. The playback is super smooth and new videos
are added frequently.
If you’re searching for a place to watch shemale creampie porn videos featuring hot performers and raw action, this is hands
down the perfect spot. Totally recommended!
Easy Canada Meds: Easy Canada Meds – Easy Canada Meds
indian pharmacy paypal: best online pharmacy india – pharmacy no prescription required
canada ed drugs Easy Canada Meds Easy Canada Meds
Easy Mex Meds: Easy Mex Meds – mexico pharmacy price list
Easy Mex Meds: best pharmacy in mexico – Easy Mex Meds
farmacia mexicana online Easy Mex Meds pharmacia mexico
http://easyindiameds.com/# top 10 pharmacies in india
Easy Mex Meds: tijuana pharmacy online – mexican pharmacy online medications
mexico pharmacy order online: Easy Mex Meds – Easy Mex Meds
Easy Canada Meds Easy Canada Meds legal canadian pharmacy online
Easy Mex Meds: Easy Mex Meds – Easy Mex Meds
top online pharmacy india: Online medicine order – buy drugs online
Fantastic! This platform has the best anal sex free Russian porn videos!
The girls take it so deep and the resolution is perfect.
At last found a place with true brutal anal action. Deep penetration and perfect creampies.
Greatest anal porn collection I’ve seen. The
scenes are so wild and the girls look incredible.
These anal sex porn videos are out of this world. Rough and super
filthy. Streaming works flawlessly.
Insane anal action! Tight asses getting pounded in the hottest way.
Totally recommended! Love it!
Easy Canada Meds Easy Canada Meds Easy Canada Meds
canada pharmacy online legit: canadian pharmacies online – Easy Canada Meds
Online medicine home delivery: Easy India Meds – worldwide pharmacy online
best rated canadian pharmacy best online canadian pharmacy Easy Canada Meds
http://easycanadameds.com/# Easy Canada Meds
top online pharmacy india: Online medicine order – no rx needed pharmacy
Easy Mex Meds: Easy Mex Meds – mexican pharma
indianpharmacy com: mail order pharmacy india – online pharmacy without scripts
Easy Mex Meds: mexico medication – affordable pharmacy
best india pharmacy indian pharmacy pharmacy no prescription required
Easy Mex Meds: pharmacy mexico city – Easy Mex Meds
Thanks for sharing. I read many of your blog posts, cool, your blog is very good.
https://easyindiameds.shop/# indian pharmacy online
Easy Mex Meds mail order pharmacy mexico Easy Mex Meds
onlinecanadianpharmacy: trustworthy canadian pharmacy – canadian pharmacy antibiotics
Easy Canada Meds: Easy Canada Meds – Easy Canada Meds
canadian online pharmacy northern pharmacy canada Easy Canada Meds
tijuana pharmacy online: is mexipharmacy legit – pharmacy in mexico city
online shopping pharmacy india: Easy India Meds – online pharmacy without scripts
mail order pharmacy mexico: Easy Mex Meds – order antibiotics from mexico
canadian drug pharmacy: legitimate canadian pharmacy online – canadian pharmacy prices
https://easyindiameds.com/# п»їlegitimate online pharmacies india
farmacia mexicana online Easy Mex Meds Easy Mex Meds
Online medicine order: top 10 online pharmacy in india – no prescription needed pharmacy
Easy Canada Meds: Easy Canada Meds – canadian 24 hour pharmacy
cheapest online pharmacy india best online pharmacy india new pharmacy online
indian pharmacy paypal: online pharmacy india – overseas pharmacy no prescription
canadian pharmacy ratings: canadianpharmacyworld – canadian world pharmacy
mexico medicine Easy Mex Meds mexican online pharmacies
Easy Canada Meds: Easy Canada Meds – canadian pharmacy ratings
http://easymexmeds.com/# purple pharmacy online ordering
I just like the helpful information you supply to your articles. I will bookmark your weblog and take a look at once more here frequently. I am moderately certain I?ll be informed lots of new stuff proper right here! Best of luck for the next!
canadian pharmacy 365: northern pharmacy canada – vipps approved canadian online pharmacy
top 10 pharmacies in india Easy India Meds new pharmacy online
Easy Canada Meds: my canadian pharmacy rx – Easy Canada Meds
indian pharmacy online Easy India Meds pharmacy online
best online pharmacy india: Easy India Meds – overseas online pharmacy
buy prescription drugs from india: india online pharmacy – top-rated online pharmacies
https://easymexmeds.com/# Easy Mex Meds
Easy Mex Meds Easy Mex Meds Easy Mex Meds
pharmacy delivery: Easy Mex Meds – Easy Mex Meds
Easy Mex Meds: mexipharmacy reviews – Easy Mex Meds
GemstoneRO Servers is one of the best Ragnarok Online private servers in 2026, offering two free RO servers: Renewal with EP21 Age of Heroes, chapter 1, chapter2 4th jobs, Doram, latest skills and mid rates, and Loki Pre-Renewal with classic gameplay, custom quests, unique gear and 100x rates. Play on PC or Android with an active global community, low-latency proxies, weekly updates and no paytowin. Join GemstoneRO and enjoy Ragnarok Online your way.
Fresh Pharm 24 us pharmacy no prescription
https://freshpharm24.com/ trustworthy online pharmacy
GemstoneRO Servers is one of the best Ragnarok Online private servers in 2026, offering two free RO servers: Renewal with EP21 Age of Heroes, chapter 1, chapter2 4th jobs, Doram, latest skills and mid rates, and Loki Pre-Renewal with classic gameplay, custom quests, unique gear and 100x rates. Play on PC or Android with an active global community, low-latency proxies, weekly updates and no paytowin. Join GemstoneRO and enjoy Ragnarok Online your way.
Fresh Pharm overseas online pharmacy
viagra fresh pharm online pharmacy no rx
https://freshpharm24.com/product/viagra worldwide pharmacy
GemstoneRO Servers is one of the best Ragnarok Online private servers in 2026, offering two free RO servers: Renewal with EP21 Age of Heroes, chapter 1, chapter2 4th jobs, Doram, latest skills and mid rates, and Loki Pre-Renewal with classic gameplay, custom quests, unique gear and 100x rates. Play on PC or Android with an active global community, low-latency proxies, weekly updates and no paytowin. Join GemstoneRO and enjoy Ragnarok Online your way.
https://freshpharm24.com/ secure medical online pharmacy
Fresh Pharm online pharmacy no prescription
generic viagra medicine online
https://freshpharm24.com/product/lipitor no rx needed pharmacy
GemstoneRO Servers is one of the best Ragnarok Online private servers in 2026, offering two free RO servers: Renewal with EP21 Age of Heroes, chapter 1, chapter2 4th jobs, Doram, latest skills and mid rates, and Loki Pre-Renewal with classic gameplay, custom quests, unique gear and 100x rates. Play on PC or Android with an active global community, low-latency proxies, weekly updates and no paytowin. Join GemstoneRO and enjoy Ragnarok Online your way.
norvasc fresh pharm no rx needed pharmacy
pharmacy worldwide pharmacy
https://freshpharm24.com/product/lipitor legitimate online pharmacy
https://freshpharm24.com/ reputable overseas online pharmacies
Fresh Pharm 24 top online pharmacy
pharmacy medicine online
https://freshpharm24.com/ online pharmacy
cialis fresh pharm pharmacy online
https://freshpharm24.com/ foreign online pharmacy
https://freshpharm24.com/ pharmacy order online
Fresh Pharm safe online pharmacies
Fresh Pharm 24 reliable online pharmacy
https://freshpharm24.com/product/lipitor п»їinternational drug mart
RateMyRagnarok is a modern Ragnarok Online private server ranking and review platform for 2026. Find the best Ragnarok private servers, RO private servers, Renewal servers, Pre-Renewal servers, low-rate, mid-rate, high-rate, custom, mobile, and classic Ragnarok Online servers. Compare rates, features, reviews, uptime, community activity, and server details. List your RO server for free and help players discover trusted Ragnarok Online private servers.
pharmacy online drugs order
https://freshpharm24.com/product/viagra medicine online
Fresh Pharm 24 us pharmacy no prescription
RateMyRagnarok is a modern Ragnarok Online private server ranking and review platform for 2026. Find the best Ragnarok private servers, RO private servers, Renewal servers, Pre-Renewal servers, low-rate, mid-rate, high-rate, custom, mobile, and classic Ragnarok Online servers. Compare rates, features, reviews, uptime, community activity, and server details. List your RO server for free and help players discover trusted Ragnarok Online private servers.
38 Park Ave FL 1, Emerson, NJ 07630
pharmacy fresh pharm medicine online
https://freshpharm24.com/ express scripts mail order pharmacy
https://freshpharm24.com/ online pharmacy
Fresh Pharm pharmacy websites
Fresh Pharm 24 legal online pharmacy
https://freshpharm24.com/product/priligy best mail order pharmacy
viagra overseas online pharmacy
Muchos expertos aseguran, el hecho de que prevenir robos en la ciudad es fundamental para la experiencia del usuario. Resulta vital analizar la infraestructura de seguridad para facilitar la movilidad diaria en las grandes metropolis.
Sitio oficial https://aa.activeboard.com/t72637774/cmo-afecta-este-fenmeno-a-la-movilidad-urbana/?page=last#lastPostAnchor
Fresh Pharm buy drugs online
https://freshpharm24.com/product/cialis best rx pharmacy online
http://stromectolvip.com/# ivermectin tablets uk
Tadalafil Tablet Cialis 20mg price Cheap Cialis
ivermectin 200mg purchase ivermectin stromectol for sale
https://sildenafilvip.shop/# Sildenafil Vip
https://sildenafilvip.shop/# Sildenafil Vip
Nice post. I used to be checking constantly this blog and I’m impressed! Very useful information specially the ultimate part 🙂 I care for such information a lot. I was seeking this certain info for a very long time. Thanks and best of luck.
ivermectin usa stromectol Vip ivermectin eye drops
http://sildenafilvip.com/# Sildenafil Vip
https://stromectolvip.com/# buy ivermectin for humans uk
ivermectin lotion cost ivermectin oral stromectol 3 mg price
Hello there! reputable online pharmacy very good website.
https://stromectolvip.online/# stromectol 3 mg price
Cheapest Sildenafil online sildenafil 50 mg price Buy generic 100mg Viagra online
https://sildenafilvip.shop/# Order Viagra 50 mg online
https://sildenafilvip.com/# Sildenafil Vip
stromectol 3mg buy stromectol canada ivermectin 9 mg
It?s hard to seek out knowledgeable folks on this subject, but you sound like you recognize what you?re speaking about! Thanks
https://stromectolvip.online/# ivermectin eye drops
https://sildenafilvip.com/# buy Viagra over the counter
ivermectin uk coronavirus stromectol Vip ivermectin 3
ivermectin tablets order stromectol tablets uk purchase stromectol online
https://cialisvip.com/# Cialis Vip
Diversos estudios confirman, que prevenir robos en la ciudad ayuda a mejorar el desarrollo del turismo. Un punto importante es las opciones de almacenamiento con el fin de potenciar el crecimiento de la ciudad en las grandes metropolis.
Informacion https://backworkclefne.bbforum.be/post542.html#542
Hello! safe online pharmacy excellent site.
https://cialisvip.com/# Cialis over the counter
Buy Tadalafil 10mg Cialis Vip Generic Tadalafil 20mg price
http://stromectolvip.com/# ivermectin 4000 mcg
https://cialisvip.online/# Cialis Vip
Generic Tadalafil 20mg price Cialis Vip Tadalafil price
ivermectin buy online stromectol Vip stromectol medication
Howdy! pharmacy technician schools online great internet site.
https://cialisvip.com/# Cialis without a doctor prescription
https://sildenafilvip.shop/# Sildenafil Vip
over the counter sildenafil sildenafil over the counter Viagra Tablet price
http://stromectolvip.com/# ivermectin new zealand
https://sildenafilvip.shop/# Sildenafil Citrate Tablets 100mg
buy cialis pill Buy Tadalafil 20mg п»їcialis generic
ivermectin price usa stromectol Vip ivermectin cost uk
http://stromectolvip.com/# generic stromectol
https://cialisvip.online/# Buy Tadalafil 20mg
ivermectin 1 buy stromectol online uk price of ivermectin
http://cialisvip.com/# Buy Tadalafil 10mg
stromectol generic stromectol Vip can you buy stromectol over the counter
https://stromectolvip.com/# stromectol ivermectin tablets
cheapest cialis Cialis without a doctor prescription Generic Cialis price
Он предлагает удобные и выгодные условия для управления капиталом.
Открой для себя новые возможности с [url=https://t.me/moneyx_tg]моней х[/url] и начни зарабатывать уже сегодня!
После неё открывается полный доступ ко всем функциям.
stromectol tab 3mg ivermectin lotion price stromectol 3mg
Caminar por una ciudad nueva con maletas a cuestas es uno de los mayores frenos para el turismo, especialmente en lugares сon tanto por ver como Buenos Aires o Ciudad de Mexico.
?Por que el equipaje limita tanto la exploracion urbana? Cuando nos liberamos del peso fisico, la movilidad urbana se vuelve mucho mas sencilla transformando un traslado tedioso en una oportunidad de paseo.
He estado siguiendo algunos hilos interesantes que tratan este tema a fondo::
Enlace http://www.klub.kobiety.net.pl/ogolny/t-qu-impacto-tienen-estas-soluciones-en-la-experiencia-del-viajeron-89135.html#post879716
?Saludos и buena ruta a todos!
https://stromectolvip.online/# ivermectin cream 5%
Buy generic 100mg Viagra online buy viagra here viagra without prescription
https://stromectolvip.online/# ivermectin 3
Tadalafil price Cialis 20mg price Generic Tadalafil 20mg price
https://sildenafilvip.shop/# Sildenafil Vip
Sildenafil Citrate Tablets 100mg Sildenafil Vip Cheap generic Viagra online
https://stromectolvip.com/# cost of ivermectin medicine
viagra without prescription Viagra tablet online best price for viagra 100mg
https://stromectolvip.com/# ivermectin price uk
From a satisfied customer: quality canadian online pharmacy – prefer pharmacies with live chat
ivermectin cream ivermectin 1 cream 45gm stromectol tablets uk
https://stromectolvip.online/# generic stromectol
Buy generic 100mg Viagra online Cheap Viagra 100mg Buy Viagra online cheap
http://stromectolvip.com/# stromectol 15 mg
I’ve learned newer and more effective things from the blog post. One other thing I have noticed is that generally, FSBO sellers will probably reject people. Remember, they might prefer never to use your providers. But if anyone maintain a comfortable, professional connection, offering support and being in contact for around four to five weeks, you will usually be capable to win a conversation. From there, a listing follows. Thank you
Generic Viagra online viagra canada Sildenafil Citrate Tablets 100mg
ivermectin oral solution stromectol Vip ivermectin 10 mg
It is the best time to make some plans for the future and it is time to be happy. I have read this post and if I could I want to suggest you few interesting things or tips. Maybe you can write next articles referring to this article. I desire to read even more things about it!
https://sildenafilvip.com/# Sildenafil Vip
Viagra generic over the counter Generic Viagra for sale Viagra without a doctor prescription Canada
Your article helped me a lot, is there any more related content? Thanks!
https://stromectolvip.com/# ivermectin 1 cream
Your article helped me a lot, is there any more related content? Thanks!
Cheap Cialis Generic Cialis price Buy Tadalafil 5mg
https://stromectolvip.com/# ivermectin drug
stromectol uk purchase oral ivermectin stromectol covid 19
When you need generic options: valtrex fast shipping – confirm shipping times upfront
My brother recommended I would possibly like this blog. He used to be totally right. This put up truly made my day. You can not believe simply how a lot time I had spent for this information! Thanks!
ivermectin otc stromectol Vip purchase ivermectin
https://liraglutideglp1.com/# buy liraglutide online
semaglutide and pcos glp-1 drugs semaglutide brand
http://liraglutideglp1.com/# victoza
liraglutide online cheap victoza buy liraglutide online
Normally I do not read article on blogs however I would like to say that this writeup very forced me to try and do so Your writing style has been amazed me Thanks quite great post
It is the best time to make some plans for the future and it’s time to be happy. I’ve read this post and if I could I wish to suggest you few interesting things or tips. Perhaps you can write next articles referring to this article. I want to read even more things about it!
рейтинг крипто БК [url=https://4dkp.forum24.ru/?1-3-0-00000155-000-0-0]рейтинг крипто БК[/url]
https://liraglutideglp1.com/# buy liraglutide online
semaglutide cheap natural semaglutide alternatives can you lose weight on rybelsus
top-rated online pharmacies trusted online pharmacy online pharmacy without scripts
Your blog is a breath of fresh air in the crowded online space. I appreciate the unique perspective you bring to every topic you cover. Keep up the fantastic work!
La libertad de movimiento es la clave para una experiencia de viaje autentica en cualquier capital, especialmente en lugares сon tanto por ver como Buenos Aires o Ciudad de Mexico.
La respuesta es simple: la comodidad permite una conexion mas profunda con el entorno. Estas herramientas modernas facilitan que cada minuto de la estadia se aproveche al maximo, evitando el cansancio innecesario y el estres de cuidar las pertenencias.
Les comparto una recopilacion de debates y articulos sobre logistica viajera::
Aqui- https://www.harderfaster.net/?sid=8804b730047ddc55077f591defaba6f5§ion=forums&action=showthread&forumid=14&threadid=349426
Nos vemos en los comentarios para debatir sobre movilidad urbana.
Your writing has a way of resonating with me on a deep level. I appreciate the honesty and authenticity you bring to every post. Thank you for sharing your journey with us.
Also I believe that mesothelioma is a exceptional form of most cancers that is generally found in those previously exposed to asbestos. Cancerous tissue form inside the mesothelium, which is a safety lining which covers many of the body’s areas. These cells generally form inside the lining of your lungs, stomach, or the sac that encircles the heart. Thanks for revealing your ideas.
https://liraglutideglp1.com/# liraglutide fast delivery
online pharmacy without scripts Victo Pharm safe online pharmacies
medstore online pharmacy reputable overseas online pharmacies shop medicine online
http://victopharm.com/# online pharmacy without scripts
I have realized that over the course of constructing a relationship with real estate homeowners, you’ll be able to get them to understand that, in each and every real estate transaction, a commission rate is paid. All things considered, FSBO sellers will not “save” the commission. Rather, they struggle to earn the commission by means of doing the agent’s task. In this, they devote their money and time to carry out, as best they can, the jobs of an agent. Those responsibilities include uncovering the home by marketing, introducing the home to prospective buyers, developing a sense of buyer emergency in order to trigger an offer, arranging home inspections, controlling qualification assessments with the loan company, supervising repairs, and assisting the closing.
крипто букмекеры [url=https://doskamarta.borda.ru/?1-5-0-00001319-000-0-0]крипто букмекеры[/url]
rybelsus costs glp-1 drugs semaglutide pill vs injection
generic liraglutide glp 1 п»їbuy liraglutide
secure medical online pharmacy worldwide pharmacy online buy drugs online
https://semaglutideglp1.shop/# what is the highest dose of semaglutide
no rx needed pharmacy Victo Pharm online pharmacy
https://liraglutideglp1.shop/# buy victoza online
крипто букмекеры [url=https://forumsilverstars.forum24.ru/?1-9-0-00000118-000-0-0]крипто букмекеры[/url]
foreign online pharmacy medicine online online pharmacy
reliable online pharmacy reputable online pharmacy no prescription legal online pharmacy
https://victopharm.shop/# pharmacy order online
рейтинг крипто БК [url=https://forumsilverstars.forum24.ru/?1-9-0-00000118-000-0-0]рейтинг крипто БК[/url]
rybelsus cost mexico glp-1 drugs compound rybelsus
safe online pharmacies Victo Pharm international pharmacy
방콕환전
http://victopharm.com/# online drugs order
liraglutide otc liraglutide pharmacy victoza generic
over the counter semaglutide glp-1 drugs for weight loss rybelsus нљЁлЉҐ
рейтинг крипто БК [url=https://mymoscow.forum24.ru/?1-5-0-00003609-000-0-0]рейтинг крипто БК[/url]
Pretty great post. I just stumbled upon your weblog and wanted to mention that I have truly loved surfing around your blog posts. After all I?ll be subscribing in your rss feed and I’m hoping you write again very soon!
http://victopharm.com/# buy drugs online
Wow that was strange. I just wrote an extremely long comment but after I clicked submit my comment didn’t appear. Grrrr… well I’m not writing all that over again. Regardless, just wanted to say great blog!
legal online pharmacy online pharmacy no prescription online pharmacy without prescription
I just could not depart your site before suggesting that I actually enjoyed the standard information a person provide for your visitors? Is gonna be back often to check up on new posts
фан спорт бк [url=https://taksafonchik.borda.ru/?1-14-0-00003165-000-0-0]фан спорт бк[/url]
liraglutide otc victoza victoza weight loss
http://victopharm.com/# best online pharmacy
legit online pharmacy pharmacy no prescription required trustworthy online pharmacy
order viagra buy viagra here – best price for viagra 100mg
Hello my loved one! I want to say that this article is awesome, nice written and come with approximately all vital infos. I would like to look more posts like this .
Buy generic 100mg Viagra online order viagra – Viagra tablet online
Cheap generic Viagra UroHealth Daily – Viagra without a doctor prescription Canada
sildenafil over the counter viagra without prescription – Buy Viagra online cheap
over the counter sildenafil UroHealth Daily – Cheap generic Viagra online
sildenafil 50 mg price generic sildenafil order viagra
Viagra online price Viagra Tablet price – Buy generic 100mg Viagra online
An additional issue is that video games are generally serious naturally with the main focus on understanding rather than leisure. Although, there is an entertainment aspect to keep children engaged, every single game is often designed to work with a specific expertise or curriculum, such as instructional math or research. Thanks for your article.
Viagra online price buy Viagra over the counter – sildenafil 50 mg price
sildenafil online UroHealth Daily – buy viagra here
태국 테더 환전소
Ive read several just right stuff here Certainly price bookmarking for revisiting I wonder how a lot effort you place to create this kind of great informative website
Sildenafil 100mg price cheap viagra – Viagra Tablet price
Viagra Tablet price best price for viagra 100mg – Order Viagra 50 mg online
Sildenafil Citrate Tablets 100mg UroHealth Daily – over the counter sildenafil
Buy Viagra online cheap UroHealth Daily – Viagra without a doctor prescription Canada
Generic Viagra for sale Sildenafil Citrate Tablets 100mg Order Viagra 50 mg online
cheapest viagra UroHealth Daily – Generic Viagra online
buy Viagra over the counter UroHealth Daily – Cheap generic Viagra online
Cheap Sildenafil 100mg Cheap generic Viagra – Viagra online price
Generic Viagra online UroHealth Daily – Viagra online price
Order Viagra 50 mg online UroHealth Daily – cheap viagra
buy viagra here UroHealth Daily – Viagra without a doctor prescription Canada
Somebody essentially help to make significantly articles Id state This is the first time I frequented your web page and up to now I surprised with the research you made to make this actual post incredible Fantastic job
Viagra without a doctor prescription Canada generic sildenafil Order Viagra 50 mg online
buy viagra here UroHealth Daily – Generic Viagra online
Premium ball gags designed for seductive restraint, playful control, and thrilling roleplay experiences. Soft comfort, adjustable fit, and bold styling help create unforgettable intimate moments filled with passion, temptation, and exciting adult fantasies for adventurous couples.
22bet ставки [url=https://astana.forum24.ru/?1-5-0-00000336-000-0-0]22bet ставки[/url]
cheap viagra UroHealth Daily – Viagra without a doctor prescription Canada
cheapest viagra Viagra online price – Generic Viagra for sale
Your blog is a breath of fresh air in the often stagnant world of online content. Your thoughtful analysis and insightful commentary never fail to leave a lasting impression. Thank you for sharing your wisdom with us.
Buy Cialis online п»їcialis generic – Cialis over the counter
https://mensrxguide.org/# cheapest cialis
Generic Cialis price Cheap Cialis – buy cialis pill
рулонные шторы купить в москве [url=https://avtomaticheskie-rulonnye-shtory50.ru]рулонные шторы купить в москве[/url]
Cialis 20mg price in USA MensRxGuide – Cheap Cialis
п»їcialis generic Buy Tadalafil 10mg Tadalafil Tablet
https://mensrxguide.org/# Cialis 20mg price in USA
Generic Cialis price cialis for sale – Cialis 20mg price in USA
заказать рулонные шторы цена [url=https://avtomaticheskie-rulonnye-shtory50.ru]https://avtomaticheskie-rulonnye-shtory50.ru[/url]
Generic Cialis without a doctor prescription MensRxGuide – Generic Cialis price
https://mensrxguide.org/# Generic Tadalafil 20mg price
Buy Cialis online Generic Cialis without a doctor prescription – cialis for sale
роликовые шторы [url=https://rulonnye-elektroshtory.ru]роликовые шторы[/url]
Buy Tadalafil 5mg Tadalafil price – Generic Cialis price
https://www.thirdcoastactivist.org/plain-radical-living-loving-and-learning-to-leave-the-planet-gracefully/
Cialis without a doctor prescription MensRxGuide – cialis for sale
http://mensrxguide.org/# buy cialis pill
This was very useful. this topic is becoming more important in 2026. Keep up the great work!
Cheap Cialis buy cialis pill – Generic Cialis price
рулонные шторы с электроприводом купить [url=https://rulonnye-elektroshtory.ru]рулонные шторы с электроприводом купить[/url]
Great article. the information shared here is very valuable. Please continue posting content like this.
Generic Cialis price Tadalafil Tablet – Cialis 20mg price in USA
안성출장마사지
cheapest cialis Buy Tadalafil 5mg – Buy Cialis online
https://mensrxguide.org/# Buy Tadalafil 5mg
рулонная штора на заказ цена [url=https://rulonnye-elektroshtory.ru]https://rulonnye-elektroshtory.ru[/url]
Buy Tadalafil 20mg MensRxGuide – Buy Cialis online
Cialis without a doctor prescription Generic Cialis price – buy cialis pill
cialis for sale MensRxGuide – Cialis without a doctor prescription
cheapest cialis Buy Tadalafil 5mg – Tadalafil Tablet
http://mensrxguide.org/# cialis for sale
рулонная штора цена [url=https://rulonnye-elektroshtory.ru]рулонная штора цена[/url]
파주출장안마
rybelsus constipation orlistat
us obesity science https://usobesityscience.org/ when will rybelsus go generic
victoza weight loss glp-1 agonists
half life of semaglutide American Metabolic Research Institute
tirzepatide https://usobesityscience.org/semaglutide-research/ cheap victoza
rybelsus for insulin resistance glp-1 agonists
вызвать капельницу от запоя [url=https://kapelnicza-ot-pokhmelya-nizhnij-novgorod-7.ru]вызвать капельницу от запоя[/url]
tirzepatide https://usobesityscience.org/glp-1-agonists/ buy victoza
how long does it take semaglutide to get out of your system liraglutide
semaglutide sodium AMRI
Excellent write-up. the step-by-step details were very helpful. Looking forward to your next post.
is rybelsus covered by medicare part d orlistat
liraglutide https://usobesityscience.org/glp-1-agonists/ how much weight can you lose on rybelsus
buy victoza online AMRI
semaglutide needles glp-1 agonists
glp-1 agonists https://usobesityscience.org/semaglutide-research/ victoza weight loss
rybelsus coupon medicare AMRI
liraglutide price orlistat
semaglutide https://usobesityscience.org/liraglutide-studies/ rybelsus savings card
victoza delivery us obesity science
liraglutide AMRI
tirzepatide https://usobesityscience.org/orlistat-clinical-review/ semaglutide oral
сколько стоит капельница от запоя [url=https://kapelnicza-ot-pokhmelya-nizhnij-novgorod-7.ru]сколько стоит капельница от запоя[/url]
semaglutide how it works glp-1 agonists
us obesity science https://usobesityscience.org/glp-1-agonists/ victoza weight loss
victoza delivery glp-1 agonists
victoza weight loss AMRI
AMRI https://usobesityscience.org/glp-1-agonists/ semaglutide
вызвать капельницу от запоя [url=https://kapelnicza-ot-pokhmelya-nizhnij-novgorod-7.ru]вызвать капельницу от запоя[/url]
what does semaglutide do American Metabolic Research Institute
cheap victoza American Metabolic Research Institute
вызвать капельницу от запоя [url=https://kapelnicza-ot-pokhmelya-nizhnij-novgorod-7.ru]вызвать капельницу от запоя[/url]
semaglutide mexico price Advancing Clinical Research in Metabolic Health and Weight Management
professional dental website design professional dental website design
semaglutide https://usobesityscience.org/orlistat-clinical-review/ glp-1
why does semaglutide cause nausea glp-1 agonists
victoza delivery tirzepatide
rybelsus patient reviews tirzepatide
tirzepatide https://usobesityscience.org/tirzepatide-analysis/ can i wait longer than 30 minutes to eat after taking rybelsus
semaglutide b12 compound liraglutide
капельница от похмелья нижний новгород [url=https://kapelnicza-ot-pokhmelya-nizhnij-novgorod-7.ru]капельница от похмелья нижний новгород[/url]
Premier porn websites provide premium content for mature
audiences. Explore secure hubs for quality and privacy.
rybelsus results Advancing Clinical Research in Metabolic Health and Weight Management
American Metabolic Research Institute https://usobesityscience.org/liraglutide-studies/ liraglutide online
glp 1 AMRI
Fantastic! This platform has the best deep anal porn!
The girls take it so deep and the resolution is unbelievable.
At last found a site with proper hardcore anal action. Ass stretching and
explosive creampies.
Best anal porn collection I’ve seen. The scenes are so wild
and the girls look incredible.
These hardcore anal clips are addictive. Hard and super filthy.
Streaming works perfectly.
Unbelievable anal action! Tight asses getting stretched in the filthiest way.
Highly recommended! My go-to site!
buy liraglutide online AMRI
прокапаться от запоя [url=https://kapelnicza-ot-pokhmelya-nizhnij-novgorod-8.ru]прокапаться от запоя[/url]
where can i get semaglutide near me liraglutide
glp-1 agonists https://usobesityscience.org/tirzepatide-analysis/ glp-1
군포출장안마
semaglutide online prescription semaglutide
liraglutide pharmacy glp-1 agonists
вызвать капельницу от запоя [url=https://kapelnica-ot-zapoya-nizhnij-novgorod-8.ru]вызвать капельницу от запоя[/url]
glp-1 agonists https://usobesityscience.org/glp-1-agonists/ victoza weight loss
semaglutide doses for weight loss liraglutide
liraglutide pharmacy liraglutide
semaglutide tirzepatide glp-1 agonists
glp-1 agonists https://usobesityscience.org/semaglutide-research/ victoza weight loss
капельница от запоя на дому цена [url=https://kapelnica-ot-zapoya-nizhnij-novgorod-8.ru]капельница от запоя на дому цена[/url]
liraglutide price liraglutide
does insurance cover semaglutide orlistat
AMRI https://usobesityscience.org/semaglutide-research/ semaglutide not losing weight
прокапаться [url=https://kapelnica-ot-zapoya-nizhnij-novgorod-8.ru]прокапаться[/url]
liraglutide fast delivery American Metabolic Research Institute
victoza glp-1 agonists
victoza glp-1 agonists
semaglutide https://usobesityscience.org/tirzepatide-analysis/ liraglutide online
вывести из запоя капельница [url=https://kapelnica-ot-zapoya-nizhnij-novgorod-8.ru]вывести из запоя капельница[/url]
rybelsus diabetes medicine Advancing Clinical Research in Metabolic Health and Weight Management
cheap victoza liraglutide
AMRI https://usobesityscience.org/glp-1-agonists/ rybelsus for
прокапаться от алкоголя на дому нижний новгород [url=https://kapelnica-ot-zapoya-nizhnij-novgorod-9.ru]прокапаться от алкоголя на дому нижний новгород[/url]
화성출장마사지
victoza delivery liraglutide
victoza delivery glp-1 agonists
American Metabolic Research Institute https://usobesityscience.org/orlistat-clinical-review/ buy liraglutide online
rybelsus assistance program American Metabolic Research Institute
капельница от запоя [url=https://kapelnica-ot-zapoya-nizhnij-novgorod-9.ru]капельница от запоя[/url]
victoza generic us obesity science
tirzepatide https://usobesityscience.org/ semaglutide prescription live forever lab
does semaglutide cause cancer American Metabolic Research Institute
Если вас интересуют [url=https://kykli.com/]шлюхи спб[/url], на нашем сайте вы найдете широкий выбор проверенных объявлений.
Индивидуалки в Санкт-Петербурге пользуются значительным спросом среди жителей и гостей города. Их услуги становятся все более популярными благодаря разнообразию и качеству. Важно понимать, что выбор индивидуалки требует внимательности и осторожности.
Каждая девушка старается
화성출장마사지
вывод из запоя капельница [url=https://kapelnica-ot-zapoya-nizhnij-novgorod-9.ru]вывод из запоя капельница[/url]
semaglutide supplement American Metabolic Research Institute
AMRI https://usobesityscience.org/liraglutide-studies/ how much is rybelsus at walmart
victoza weight loss semaglutide
rybelsus contraindications semaglutide
наркологический стационар санкт петербург [url=https://narkologicheskij-staczionar-sankt-peterburg-10.ru]наркологический стационар санкт петербург[/url]
п»їbuy liraglutide American Metabolic Research Institute
화성출장안마
semaglutide https://usobesityscience.org/glp-1-agonists/ do you lose weight on rybelsus
liraglutide orlistat
кодирование от алкоголизма стационар [url=https://narkologicheskij-staczionar-sankt-peterburg-10.ru]кодирование от алкоголизма стационар[/url]
liraglutide orlistat
AMRI https://usobesityscience.org/semaglutide-research/ who manufactures rybelsus
liraglutide pharmacy liraglutide
liraglutide otc Advancing Clinical Research in Metabolic Health and Weight Management
how many mg is 40 units of semaglutide glp-1 agonists
tirzepatide https://usobesityscience.org/semaglutide-research/ why does semaglutide cause nausea
Fantastic! This website is truly top-notch! The selection of shemale porn videos is unbelievable – tons of sexy trans girls in premium scenes.
The streaming is butter-smooth and new content are added all the time.
If you’re searching for a place to watch shemale porn videos featuring beautiful
performers and real action, this is without a doubt the ultimate spot.
Highly recommended!
Also visit my blog post; nude sites sex
наркологический стационар [url=https://narkologicheskij-staczionar-sankt-peterburg-10.ru]наркологический стационар[/url]
does semaglutide work American Metabolic Research Institute
can you break rybelsus in half orlistat
semaglutide https://usobesityscience.org/orlistat-clinical-review/ victoza generic
наркологический стационар в спб [url=https://narkologicheskij-staczionar-sankt-peterburg-10.ru]наркологический стационар в спб[/url]
https://amoxilidari.com/clinical-dosing-protocols/# buy cheap amoxicillin online
can i buy amoxicillin over the counter in australia Amoxil buy cheap amoxicillin online
purchase amoxicillin online without prescription AmoxilIdari amoxicillin 500 mg price
https://amoxilidari.com/amoxil-vs-generic/# amoxicillin order online
https://amoxilidari.com/amoxil-vs-generic/# amoxicillin without prescription
стационар наркологический санкт петербург [url=https://narkologicheskij-staczionar-sankt-peterburg-10.ru]стационар наркологический санкт петербург[/url]
Toonaangevende pornosites bieden veilige en premium inhoud voor volwassenen. Ontdek
betrouwbare hubs voor een kwaliteitservaring.
amoxicillin medicine IDARI amoxicillin 30 capsules price
https://amoxilidari.com/# how to get amoxicillin
https://ivermectiniaar.shop/# ivermectin canada
ivermectin 1 cream 45gm Clinical Pharmacology and Safety Profiles of Stromectol ivermectin iv
amoxicillin 500mg without prescription Infectious Disease & Antimicrobial Research Institute amoxicillin online purchase
стационар наркологический санкт петербург [url=https://narkologicheskij-staczionar-sankt-peterburg-10.ru]стационар наркологический санкт петербург[/url]
https://neurontinnnprc.shop/# gabapentin cognitive impairment
https://neurontinnnprc.shop/# gabapentin cognitive impairment
how much is amoxicillin prescription Amoxil amoxicillin capsules 250mg
наркологический стационар спб [url=https://narkologicheskij-staczionar-sankt-peterburg-11.ru]наркологический стационар спб[/url]
https://ivermectiniaar.com/stromectol-dosage-protocols/# stromectol tablets buy online
ivermectin gel Clinical Pharmacology and Safety Profiles of Stromectol stromectol 3mg tablets
https://amoxilidari.com/sourcing-and-telemedicine/# how much is amoxicillin
amoxicillin 500mg buy online uk Amoxil amoxicillin generic
Amazing! This website is truly top-notch! The collection of shemale porn videos is massive –
so many stunning trans girls in crystal-clear scenes.
The playback is super smooth and new content are added every day.
If you’re looking to watch shemale fucks girl porn videos featuring beautiful performers and
intense action, this is definitely the ultimate spot.
Strongly recommended!
https://neurontinnnprc.com/# gabapentin spinal surgery
ivermectin canada Institute for Clinical Pharmacology & Safety buy ivermectin uk
https://amoxilidari.com/sourcing-and-telemedicine/# amoxicillin 500mg capsule
нарколог стационар спб [url=https://narkologicheskij-staczionar-sankt-peterburg-11.ru]нарколог стационар спб[/url]
where can i get gabapentin gabapentin cognitive impairment gabapentin actavis bivirkninger
https://amoxilidari.com/amoxil-vs-generic/# amoxicillin medicine
https://amoxilidari.com/sourcing-and-telemedicine/# buy amoxicillin 500mg usa
amoxicillin for sale Infectious Disease & Antimicrobial Research Institute amoxicillin tablets in india
buy amoxicillin canada AmoxilIdari generic amoxicillin
наркологический стационар в санкт петербурге [url=https://narkologicheskij-staczionar-sankt-peterburg-11.ru]наркологический стационар в санкт петербурге[/url]
https://amoxilidari.com/amoxil-vs-generic/# how to get amoxicillin
https://amoxilidari.com/sourcing-and-telemedicine/# price of amoxicillin without insurance
ivermectin drug Ivermectin ivermectin lotion cost
https://mexicaredirect.com/# MexiCare Direct
progreso, mexico pharmacy online MexiCare Direct MexiCare Direct
нарколог стационар [url=https://narkologicheskij-staczionar-sankt-peterburg-11.ru]нарколог стационар[/url]
Easy North RX: buy canadian drugs – online pharmacy canada
indian pharmacy paypal: Flexi Meds India – pharmacy online
https://mexicaredirect.shop/# mexico prescriptions
canadian pharmacy 24: best rated canadian pharmacy – canadian pharmacy scam
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
Easy North RX: Easy North RX – safe reliable canadian pharmacy
наркологический стационар в санкт петербурге [url=https://narkologicheskij-staczionar-sankt-peterburg-11.ru]наркологический стационар в санкт петербурге[/url]
Увеличьте видимость вашего бизнеса в интернете с помощью качественного
[url=https://msk.mihaylov.digital/vnutrennjaja-optimizacija-sajta/]https://msk.mihaylov.digital/vnutrennjaja-optimizacija-sajta/[/url]
Первый этап SEO — анализ целевой аудитории и выбор ключевых слов.
https://mexicaredirect.shop/# mexico meds
Easy North RX online pharmacy canada canadian online pharmacy reviews
legit canadian pharmacy online: cheap canadian pharmacy online – drugs from canada
дезинфекция в Санкт-Петербурге
[url=https://dezinfection-v-spb.click/]https://dezinfection-v-spb.click/[/url]
http://fleximedsindia.com/# п»їlegitimate online pharmacies india
кодирование от алкоголизма стационар [url=https://narkologicheskij-staczionar-sankt-peterburg-11.ru]кодирование от алкоголизма стационар[/url]
best canadian pharmacy to order from: Easy North RX – Easy North RX
MexiCare Direct: mexican pharmacy prices – online mexican pharmacy
https://fleximedsindia.shop/# indian pharmacy
MexiCare Direct MexiCare Direct can i buy meds from mexico online
canada pharmacy store: Easy North RX – reliable canadian pharmacy reviews
top 10 online pharmacy in india: Flexi Meds India – legal online pharmacy
https://fleximedsindia.shop/# indian pharmacies safe
canadian pharmacy meds reviews: canadian pharmacy 24 com – Easy North RX
https://easynorthrxs.com/# Easy North RX
indian pharmacy online: Flexi Meds India – п»їinternational drug mart
cross border pharmacy canada Easy North RX canadian pharmacy 24
Easy North RX: vipps approved canadian online pharmacy – Easy North RX
https://fleximedsindia.com/# indian pharmacy
Online medicine order: Flexi Meds India – no prescription pharmacy paypal
п»їlegitimate online pharmacies india: top 10 pharmacies in india – п»їinternational drug mart
https://mexicaredirect.com/# best mexican pharmacy online
canadian pharmacy 24h com: canadian pharmacy com – canadian pharmacy king reviews
MexiCare Direct mexican pharmacies that ship purple pharmacy online
http://easynorthrxs.com/# Easy North RX
indian pharmacies safe: best online pharmacy india – online pharmacy
mexico pharmacy order online: online pharmacy in mexico – mexico prescriptions
https://fleximedsindia.com/# online pharmacy india
Easy North RX: Easy North RX – Easy North RX
world pharmacy india Flexi Meds India online drugs order
Your point of view caught my eye and was very interesting. Thanks. I have a question for you. https://accounts.binance.com/register/person?ref=IHJUI7TF
наркологическая клиника [url=https://narkologicheskaya-pomoshh-voronezh-11.ru]наркологическая клиника[/url]
https://easynorthrxs.shop/# Easy North RX
drugs from canada: Easy North RX – canadian pharmacies shipping to usa
india pharmacy: Flexi Meds India – pharmacy no prescription required
http://mexicaredirect.com/# medication from mexico
помощь наркозависимым [url=https://narkologicheskaya-pomoshh-voronezh-11.ru]https://narkologicheskaya-pomoshh-voronezh-11.ru[/url]
indian pharmacy: best online pharmacy india – online pharmacy no prescription
pet meds without vet prescription canada: Easy North RX – Easy North RX
indianpharmacy com Online medicine home delivery online pharmacy without scripts
https://fleximedsindia.shop/# top online pharmacy india
canadian drugs: Easy North RX – Easy North RX
лечение наркомании анонимно [url=https://narkologicheskaya-pomoshh-voronezh-11.ru]https://narkologicheskaya-pomoshh-voronezh-11.ru[/url]
http://fleximedsindia.com/# top 10 online pharmacy in india
Easy North RX: northwest canadian pharmacy – Easy North RX
reputable indian pharmacies Flexi Meds India shop medicine online
https://mexicaredirect.com/# pharmacy mexico city
Easy North RX: Easy North RX – Easy North RX
MexiCare Direct: can i order online from a mexican pharmacy – MexiCare Direct
https://easynorthrxs.com/# Easy North RX
Easy North RX: Easy North RX – Easy North RX
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
canadian pharmacy tampa canadian drugstore online Easy North RX
http://fleximedsindia.com/# Online medicine order
india online pharmacy: top online pharmacy india – pharmacy online
MexiCare Direct: farmacia mexicana online – pharmacy delivery
скорая наркологическая помощь [url=http://narkologicheskaya-pomoshh-voronezh-13.ru]http://narkologicheskaya-pomoshh-voronezh-13.ru[/url]
http://easynorthrxs.com/# canadian world pharmacy
online pharmacy india: Online medicine order – foreign online pharmacy
indianpharmacy com: top online pharmacy india – worldwide pharmacy online
В Москве существует множество автосервисов, специализирующихся на Тойота. Специалисты готовы осуществлять ремонт и обслуживание ваших автомобилей.
Если вам нужен качественный и надежный [url=https://servis-toyota-moskva.su/remont-toyota-v-moskve/] автосервис Toyota в Москве[/url], мы предлагаем широкий спектр услуг для вашего автомобиля.
Работа с автомобилями этой марки требует особого подхода. Каждый механик проходит специальное обучение и сертификацию.
В автосервисе установлено современное оборудование. Наличие современного оборудования существенно упрощает процесс диагностики.
Наш автосервис обеспечивает надежность и долговечность вашего автомобиля. Ваше доверие для нас — наивысшая награда.
https://fleximedsindia.com/# india pharmacy mail order
medication from mexico: MexiCare Direct – mexico prescription online
наркология круглосуточная [url=http://narkologicheskaya-pomoshh-voronezh-13.ru]http://narkologicheskaya-pomoshh-voronezh-13.ru[/url]
https://mexicaredirect.shop/# MexiCare Direct
canadianpharmacymeds com: canadian discount pharmacy – best canadian pharmacy online
pharmacia mexico: reliable rx pharmacy – hydrocodone mexico pharmacy
наркологический центр воронеж [url=http://narkologicheskaya-pomoshh-voronezh-13.ru]наркологический центр воронеж[/url]
https://fleximedsindia.com/# indian pharmacy paypal
77 canadian pharmacy canadian pharmacy king reviews canadian pharmacy no scripts
canadian pharmacy cheap: vipps approved canadian online pharmacy – Easy North RX
legitimate canadian pharmacy: canada pharmacy world – Easy North RX
http://mexicaredirect.com/# can i order online from a mexican pharmacy
наркологическая клиника в воронеже [url=https://www.narkologicheskaya-pomoshh-voronezh-13.ru]наркологическая клиника в воронеже[/url]
MexiCare Direct: medication in mexico – mexican online pharmacies
http://fleximedsindia.com/# online shopping pharmacy india
mail order pharmacy india indian pharmacy overseas online pharmacy
trustworthy canadian pharmacy: Easy North RX – canadian pharmacy ratings
MexiCare Direct: MexiCare Direct – best mexican pharmacy
лечение алкоголизма в воронеже [url=http://narkologicheskaya-pomoshh-voronezh-13.ru]лечение алкоголизма в воронеже[/url]
http://easynorthrxs.com/# Easy North RX
mail order pharmacy india: india pharmacy – medicine online order
recommended canadian pharmacies: Easy North RX – legitimate canadian mail order pharmacy
https://mexicaredirect.com/# MexiCare Direct
Easy North RX: canadian drug stores – pharmacy rx world canada
MexiCare Direct the purple pharmacy mexico mexican pharmacy ship to usa
https://fleximedsindia.shop/# top online pharmacy india
indian pharmacy: india online pharmacy – buy drugs online
MexiCare Direct: mexico online farmacia – MexiCare Direct
В Москве существует множество автосервисов, специализирующихся на Тойота. Специалисты готовы осуществлять ремонт и обслуживание ваших автомобилей.
Если вам нужен качественный и надежный [url=https://servis-toyota-moskva.su/remont-toyota-v-moskve/] автосервис Toyota в Москве[/url], мы предлагаем широкий спектр услуг для вашего автомобиля.
Для Тойота необходим высокий уровень квалификации. Мастера сервиса постоянно повышают свою квалификацию для качественного обслуживания.
Техническое оснащение сервиса соответствует самым высоким стандартам. Благодаря этому, мы можем гарантировать качество выполняемых работ.
Вы получите качественное и профессиональное обслуживание вашего автомобиля. Мы ценим каждого клиента и стремимся к его удовлетворенности.
I have been browsing online more than three hours today yet I never found any interesting article like yours It is pretty worth enough for me In my view if all website owners and bloggers made good content as you did the internet will be a lot more useful than ever before
поставить капельницу от алкоголя [url=https://kapelnicza-ot-pokhmelya-samara-28.ru]поставить капельницу от алкоголя[/url]
Your blog is a testament to your dedication to your craft. Your commitment to excellence is evident in every aspect of your writing. Thank you for being such a positive influence in the online community.
http://fleximedsindia.com/# top 10 online pharmacy in india
pharmacy website india: cheapest online pharmacy india – best rx pharmacy online
canadian online pharmacy no prescription Easy North RX the canadian drugstore
Hi my loved one I wish to say that this post is amazing nice written and include approximately all vital infos Id like to peer more posts like this
Your blog is a constant source of inspiration for me. Your passion for your subject matter shines through in every post, and it’s clear that you genuinely care about making a positive impact on your readers.
MexiCare Direct: MexiCare Direct – MexiCare Direct
https://easynorthrxs.com/# pharmstore canada
Easy North RX: Easy North RX – pharmacy wholesalers canada
капельница от алкоголя на дому [url=https://kapelnicza-ot-pokhmelya-samara-28.ru]капельница от алкоголя на дому[/url]
https://mexicaredirect.shop/# purple pharmacy online ordering
canadian online pharmacy: canadianpharmacymeds com – canada drugs online reviews
MexiCare Direct: mexican rx – best online mexican pharmacy
top online pharmacy india Flexi Meds India online pharmacies
капельница от алкоголя на дому самара недорого [url=https://kapelnicza-ot-pokhmelya-samara-28.ru]капельница от алкоголя на дому самара недорого[/url]
https://fleximedsindia.shop/# best online pharmacy india
MexiCare Direct: meds from mexico – MexiCare Direct
вывести из запоя капельница на дому [url=https://kapelnicza-ot-pokhmelya-samara-28.ru]вывести из запоя капельница на дому[/url]
https://mexicaredirect.shop/# MexiCare Direct
indianpharmacy com: india pharmacy – п»їinternational drug mart
pharmacy in mexico best mexican pharmacy tijuana pharmacy online
https://easynorthrxs.shop/# Easy North RX
Easy North RX: Easy North RX – canadian pharmacies shipping to usa